Primary breast lymphoma (PBL) is a clinicopathological entity characterized by the appearance of a unilateral breast mass of months of evolution, infrequently accompanied by signs of skin edema, retraction, erythema and nipple involvement. This rare situation is especially observed during pregnancy or postpartum, suggesting that tumor growth is influenced by hormonal stimulation, although its association with other processes such as antecedent autoimmune diseases have been documented.1
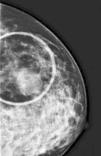
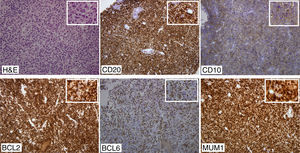
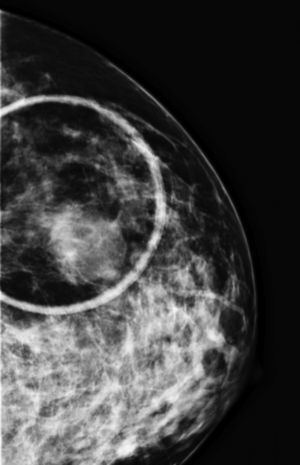
We report the case of a 46-year-old female, with no medical history of interest, who consulted due to the appearance of a 4-cm tumor in the left breast of six months of evolution. We proceeded with the study, making radiological imaging (mammogram and magnetic resonance) and histopathological investigations. The examinations conducted, including blood count, biochemistry, serologies, and tumor markers, were normal highlighting slightly elevated ¿2-microglobulin levels (2.9mg/L). Mammography and magnetic resonance findings were suggestive of breast cancer. Histological examination showed a tumor composed of a large-sized cell infiltrate, with scarce cytoplasm, irregular nuclear membrane, split cells with prominent nucleoli, and numerous mitoses. The immunohistochemical study showed positivity for tumor populations CD19, CD20, CD79a, PAX-5, bcl-2, bcl-6 and MUM-1 and focally for CD10 and negativity for cyclin D1 and CD38 (Figure 1). Ki 67 was 80%. Given the combination of clinical, histopathological, and immunohistochemical findings, a diagnosis of primary diffuse large B-cell non-Hodgkin lymphoma was established, warranting an extended study with a cervico-thoraco-abdomino-pelvic scan and bone marrow biopsy to rule out lymphadenopathies and bone marrow infiltration. With the diagnosis of primary diffuse large B-cell non-Hodgkin lymphoma, chemotherapy was established using the R-CHOP scheme (rituximab, cyclophosphamide, adriamycin, vincristine and prednisone).
PBL is a rare entity in everyday medical practice. Initially described by Gross in 1880, it is about 0.4–0.5% of all malignant breast tumors and 0.38–0.70% of non-Hodgkin lymphomas,2 with the most common subtype being diffuse large B-cell non-Hodgkin lymphoma. It is characterized by the appearance of a unilateral breast mass particularly in the upper quadrant of the right side. The incidence increases with age. Patients with PBL infrequently present with signs of skin edema, retraction, erythema, and nipple involvement. Although its etiology is unknown, its association with different processes, among which are estrogen and autoimmune diseases,3 has been described; none of these associations were found in our patient. Other entities that present with similar breast swelling and symptoms should be considered in the differential diagnosis. To do this, clinicians rely on a detailed anamnesis, and complementary analytical and imaging studies (Figure 2). The diagnosis, regardless of the clinical data provided by the patient and the exclusion of other entities, is established when a consistent histological pattern is demonstrated.
The authors declare no conflicts of interest.