The Brazilian elderly population is growing exponentially, making prevention and treatment of chronic diseases a priority in this age group. Anemia in older adults is underdiagnosed, undervalued and associated with high morbimortality.
ObjectiveTo assess the prevalence of anemia in the elderly residents of a long-term care institution and to correlate this with individual patient history, the use of polypharmacy and mortality.
MethodA retrospective study was carried out of data extracted from medical records of patients treated in 2014 at the Hospital Geriátrico e de Convalescentes Dom Pedro II under the Preventive Actions Program.
ResultsData were collected from 88 female (48%) and 95 male (52%) elderly residents at a long-term care institution. Patient ages ranged from 60 to 102 years with a mean age of 76.3 years. Overall, 76 participants were diagnosed with anemia, representing 41% of the sample. Of those diagnosed, 35 were women (46%) and 41 were men (54%).
ConclusionAnemia in the elderly is a clinical condition associated with increased morbimortality. However, the disorder remains underdiagnosed, resulting in higher risks for older adults. The present study found 76 patients with anemia among the 183 residents at the long-term care institution. The patient profile of this population with anemia is non-smokers, male, aged between 70 and 79 years, with normochromic/normocytic anemia and taking multiple medications.
The elderly population in Brazil, defined by the World Health Organization (WHO) as individuals over the age of 60 years, is growing rapidly. The latest census carried out in 2010 recorded a total population of 190,732,694, of whom 19,090,597 were over 60 years of age; the population projection for 2017 is 207,115,436 individuals.1 The same census showed that there were 4,771,436 elderly in São Paulo State, representing 24.9% of the total Brazilian elderly population.1
Anemia can be defined as a decrease in the hematocrit or hemoglobin (Hb) concentration, or red blood cell (RBC) count. This condition can affect the oxygen-carrying capacity, leading to insufficient oxygen to meet physiologic needs. Anemia is the most common blood disorder in the elderly.2–4
Measures that estimate circulating RBC mass are used to diagnose anemia. The exams required to diagnose the condition vary depending on level of clinical suspicion, but may include: whole blood count, iron studies (serum iron, total iron binding capacity, serum ferritin), serum vitamin B12 level, serum folate level, and a bone marrow exam.1,2,5,6
Anemia is considered an independent risk factor for various geriatric conditions, including frailty syndrome, functional decline, cognitive decline, increased morbidity, increased hospitalization and higher mortality. Therefore, its outcome reduces the quality of life and independence of the elderly population.2,7–10
In 2015 in Brazil, there were a total of 2433 hospital admissions of avoidable cases of anemia in elderly patients.11,12
According to the WHO, anemia in women is classified as mild when Hb values are between 11.0 and 11.9g/dL, moderate for Hb from 8.0 to 10.9g/dL and severe for levels under 8mg/dL. The only difference for men is the value for mild anemia, which is defined as Hb of between 11.0 and 12.9g/dL.
Anemia in the elderly can be classified under three main categories that may be concomitant: nutritional deficiency (iron, folate or vitamin B12), anemia of inflammation or of chronic disease, and unexplained anemia.1
The aim of this study was to assess the prevalence of anemia in the elderly patients of a long-term care institution and to correlate this with individual patient history, polypharmacy and mortality.
MethodThe Hospital Geriátrico e de Convalescentes Dom Pedro II is a long-term institution that was founded more than 100 years ago. It houses patients with some degree of dependency and without the possibility of living alone, who do not have social support or whose families are unable to provide adequate and dignified care for them.
A retrospective study was carried out of data extracted from the medical records of patients treated in 2014 by the institution under the Preventive Actions Program (PAP). The medical records of the institution contain a standardized geriatric evaluation completed in the first evaluation of the patient.
The goals of the PAP are to define and routinely apply standardized protocols in institutionalized patients to prevent high impact and/or highly prevalent diseases in the elderly at long-term care institutions. The PAP patients were chosen randomly from the total number of long-term institutional residents with each physician at the institution being responsible for the evaluation of ten patients. The program started in March 2009 and addressed four circumstances:
- 1.
Primary prevention entails actions aimed at avoiding diseases by tackling causal factors, such as vaccines, adequate nutrition and oral health.
- 2.
Secondary prevention encompasses a group of actions aimed at reducing the prevalence of diseases through early diagnosis and treatment with screening exams, including the complete blood count (CBC).
- 3.
Tertiary prevention comprises actions aimed at reducing the disabilities caused by sequelae of diseases.
- 4.
Quaternary prevention seeks to avert iatrogenic events and hospital admission-related complications.
The following variables, based on information previously collected by the PAP, were analyzed: name, age, gender, ethnicity, duration of institutional care, comorbidities, lifestyle, substance use and medications being taken. This information was correlated with the prevalence and type of anemia of the residents.
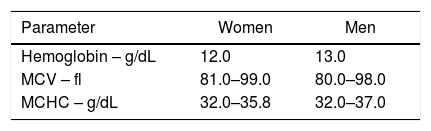
The definition of anemia for the present study was based on the WHO criteria and included analysis of the RBC parameters, mean corpuscular volume and mean corpuscular hemoglobin concentration (Table 1). The diagnosis of anemia in patients was performed using the CBC performed during the secondary prevention measures.
The inclusion criteria were patients aged 60 years or older admitted to the institution before January 2014 and assessed by the PAP in 2014.
ResultsData were collected for 183 residents at the long-term care institution; 88 women (48%) and 95 men (52%). Their ages ranged from 60 to 102 years with a mean of 76.3 years. On stratifying participants by age group, 50 (27.3%) were from 60 to 69 years old, 62 (33.87%) were from 70 to 79 years old, 59 (32.24%) were from 80 to 89 years old and 12 (6.56%) were over 90 years of age.
There were 18 (9.84%) deaths among the participants during the course of 2014, nine (50%) of whom had anemia.
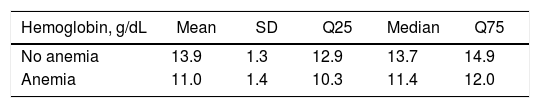
Overall, 76 of the residents were diagnosed with anemia, representing 41% of the sample. The group diagnosed with anemia comprised 36 women (47.4%) and 40 men (52.6%). Table 2 shows the descriptive measures for Hb in patients with and without anemia. The 95% confidence intervals related to Hb were 10.69–11.3 and 13.67–14.16 for patients with and without anemia, respectively.
Descriptive measures for hemoglobin levels in patients with and without anemia.
| Hemoglobin, g/dL | Mean | SD | Q25 | Median | Q75 |
|---|---|---|---|---|---|
| No anemia | 13.9 | 1.3 | 12.9 | 13.7 | 14.9 |
| Anemia | 11.0 | 1.4 | 10.3 | 11.4 | 12.0 |
Q25: first quartile (25th percentile); Q75: third quartile (75th percentile); SD: Standard Deviation.
p-value=<0.001.
Analysis of the type of anemia showed that 46 (60.53%) patients had normochromic/normocytic anemia (22 women and 24 men), 14 (18.42%) had hypochromic/microcytic anemia (8 women and 6 men), six (7.89%) had normochromic/microcytic anemia (1 woman and 5 men), nine (11.84%) had normochromic/macrocytic anemia (6 women and 3 men) and only one (1.32%) man had hypochromic/normocytic anemia.
A total of 135 (73.77%) participants were taking multiple medications. Of this group, 62 (46.0%) anemic patients were found to be taking multiple medications. A total of 14 patients were diagnosed with anemia but were not taking multiple medications. Among the patients with both anemia and polypharmacy, 37 (59.68%) had normochromic/normocytic anemia (20 women and 17 men), 11 (17.74%) had hypochromic/microcytic (6 women and 5 men), six (9.68%) had normochromic/microcytic (1 women and 5 men), seven had normochromic/macrocytic (6 women and 1 men) and only one men (1.61%) had hypochromic/normocytic anemia.
The main classes of medications being taken by the anemic patients taking multiple medications, in decreasing order of prevalence, were: antihypertensive drugs (77.4%) in particular captopril and hydrochlorothiazide, proton pump inhibitors (omeprazole – 66.1%), laxatives (lactulose – 50%), statins (simvastatin – 45.1%) and antiplatelet drugs (acetylsalicylic acid – 40.3%).
Of the 183 (15.3%) patients analyzed, 28 were smokers (6 women and 22 men) with only eight of the smokers having anemia (1 woman and 7 men).
Fifty-one anemic patients were White (26 women and 25 men), 12 were Black (5 women and 7 men), two were Asian (both men), and 11 were Mulattos (4 women and 7 men).
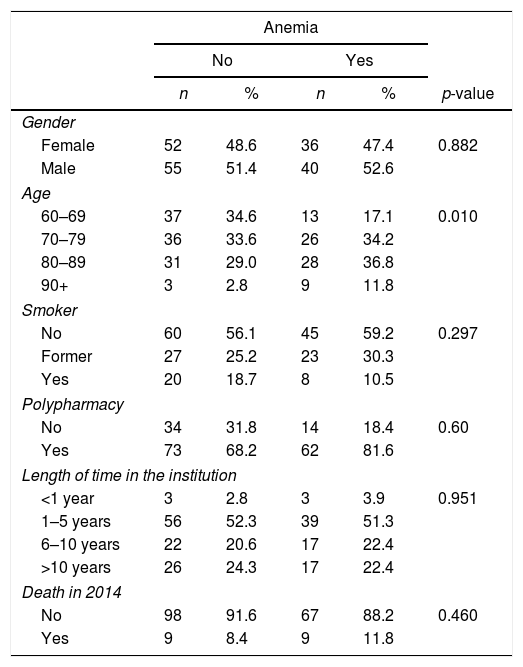
A summary of the data obtained in this work is summarized in Table 3.
Absolute and percentage frequencies for categorical variables in patients with and without anemia, and p-value (Fisher's exact test).
| Anemia | |||||
|---|---|---|---|---|---|
| No | Yes | ||||
| n | % | n | % | p-value | |
| Gender | |||||
| Female | 52 | 48.6 | 36 | 47.4 | 0.882 |
| Male | 55 | 51.4 | 40 | 52.6 | |
| Age | |||||
| 60–69 | 37 | 34.6 | 13 | 17.1 | 0.010 |
| 70–79 | 36 | 33.6 | 26 | 34.2 | |
| 80–89 | 31 | 29.0 | 28 | 36.8 | |
| 90+ | 3 | 2.8 | 9 | 11.8 | |
| Smoker | |||||
| No | 60 | 56.1 | 45 | 59.2 | 0.297 |
| Former | 27 | 25.2 | 23 | 30.3 | |
| Yes | 20 | 18.7 | 8 | 10.5 | |
| Polypharmacy | |||||
| No | 34 | 31.8 | 14 | 18.4 | 0.60 |
| Yes | 73 | 68.2 | 62 | 81.6 | |
| Length of time in the institution | |||||
| <1 year | 3 | 2.8 | 3 | 3.9 | 0.951 |
| 1–5 years | 56 | 52.3 | 39 | 51.3 | |
| 6–10 years | 22 | 20.6 | 17 | 22.4 | |
| >10 years | 26 | 24.3 | 17 | 22.4 | |
| Death in 2014 | |||||
| No | 98 | 91.6 | 67 | 88.2 | 0.460 |
| Yes | 9 | 8.4 | 9 | 11.8 | |
One of the objectives of the present study was to differentiate the causes of anemia in the population studied. However, because the study was retrospective, based on data from medical records, some key information required to differentiate the etiology of the anemia was unavailable, precluding classification by anemia type. Considering a level of significance of 5%, a statistically significant association was observed only for age.
The North American National Health and Nutrition Examination Survey (NHANES III) conducted in 2013 and 2014 is part of the National Center for Health Statistics program responsible for producing statistics in the USA. The study revealed that 10.2% of women and 11.0% of men over 60 years of age from the community had anemia. Among the over 85-year-old patients, anemia rates were 20.1% for women and 26.1% for men.
A study of community-dwelling elderly of 60 years or older carried out in the city of Bambuí, in Minas Gerais, found an overall prevalence of anemia of 3.8% with rates for men and women of 4.6% and 3.3%, respectively.13
Macêdo et al.14 performed a study at a long-term care facility in the Federal District of Brasília and found an overall prevalence of anemia of 29.7% with rates of 26.1% for women and 38.9% for men. The most common type of anemia was normochromic and normocytic, accounting for 64.7% of the cases assessed. In the current study, a higher rate was found for this type of anemia, which was also more prevalent in men. However, in this population the percentage of patients with anemia was significantly higher, probably due to sociodemographic differences of the populations studied.
In 2015, a review on the prevalence and etiology of anemia in older adults was carried out. The results of the studies analyzed showed a higher prevalence of anemia in hospitalized and institutionalized elderly.15
Unlike most investigations, the present study involved an institutionalized population and found an overall prevalence of anemia of 41% of the sample, with 46% of cases being women and 54% being men. This disparity between the data collected in the present study and those of previous studies is due to the fact that institutionalized patients are generally frailer than community-dwelling elderly and they have a higher number of comorbidities and take more medications.1,16
Among participants who died in 2014, 50% had anemia. This data corroborates the literature that reports a higher mortality rate among patients with this pathology.2,7–10
ConclusionAnemia in the elderly is a clinical condition associated with increased morbimortality but remains underdiagnosed, resulting in a greater risk for older adults. Therefore, elderly patients suspected of having anemia should be investigated and treated.
The present study found a greater prevalence of anemia than in the literature consulted, probably resulting from the type of patients admitted to this long-term institution. The profile of patients with anemia in this institution is non-smokers, male, with ages ranging between 70 and 79 years, with normochromic/normocytic anemia, and taking multiple medications.
The most frequent type of anemia found in the current study (normochromic/normocytic) may indicate that the main cause of anemia is chronic diseases, but due to lack of available data, this hypothesis cannot be confirmed.
Although a prominent theme, studies of anemia in institutionalized populations are scarce and further research on the subject is warranted.
Conflict of interestThe authors declare no conflicts of interest.