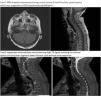
Neurotoxicity is a serious but incompletely understood complication of CAR T-cell therapy. here we highlight presentation and diagnostic challenges of non-CNS CAR T-cell therapy complication.
Case seriesCase 1: A 43-year-old female with relapsed DLBCL stage IVB without CNS involvement underwent Axi-Cel CAR T-cell therapy, developing grade I CRS responded to tocilizumab. On day +15, developed diplopia and 6th nerve palsy MRI suggestive CNS lymphomatous infiltration, managed with dexamethasone and intrathecal MTX with a PET scan on day 30 showing CMR. Subsequently, she had limbs weakness with EMG/NCS confirming polyradiculopathy CSF showing high protein but negative for infection, malignant cells and autoimmune. Treatment included methylprednisolone, plasmapheresis, and IVIG, leading to slight improvement. Day 60 PET-CT revealed cervical and lumbar nerve roots neuritis, and by day 90, biopsy-confirmed disease relapse. She had partial response to glofitamab, unfortunately, she passed away four months post-CAR T-cell therapy.
Case 2: A 38-year-old male with primary refractory stage III DLBCL received Axi-Cel after lymphodepletion with Flu/Cy. On day +1, grade I CRS developed and was treated with tocilizumab and dexamethasone. By day +4, he exhibited ICANS grade IV with confusion and seizures, managed with methylprednisolone, anakinra, and lorazepam. CSF showed high protein but no infection or malignant cells. MRI suggested viral encephalitis, and acyclovir was started. Extubated on day +8, but showed lower limb weakness (0/5 power) and urinary retention. Spinal MRI showed intramedullary T2 changes. IVIG was given on day +11, and physical therapy started. By day +16, he could stand; MRI normalized by day +29. PET-CT on day +32 showed a very good partial response. The patient was able to walk and discharged on day +39 with ongoing recovery.
Case 3: A 36-year-old male with CML transformed to B-cell ALL with CNS involvement refractory to triple IT chemotherapy received IT thiotepa, complicating with lower limb weakness and sphincter loss. NCS confirmed L5 radiculopathy; MRI and CSF were negative for blasts or CNS disease. Post-Brexu-cel infusion (day +5 to +7), he developed CRS grade I, treated with Tocilizumab, followed by worsening lower limb weakness and sensory loss. MRI revealed new cauda equina leptomeningeal enhancement; NCS confirmed bilateral polyradiculopathy. CSF showed high protein but no blasts or infections. IVIG, methylprednisolone, anakinra and IT MTX-hydrocortisone improved symptoms. MRD assessment on day +30 was negative repeated MRI brain and spine showed resolution of leptomeningeal enhancement.
ConclusionWith the increasing use of CAR T-cell therapy, rare side effects, such as sensory-motor polyradiculopathy, are emerging. These cases underscore the challenges of diagnosing and managing non-CNS neurotoxicity. Early recognition, tailored interventions, and multidisciplinary care are vital, while further research is needed to better understand mechanisms and improve patients’ outcomes.