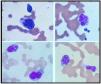
A 59-year-old male presented with increased fatiguability and features of renal insufficiency. His routine work up showed raised urea (317mg/dL), creatinine (3.9mg/dL), sodium (155 mEq/L) and LDH (1773 U/L). Hemogram revealed anemia (Hemoglobin=7.5g/dL) and thrombocytopenia (Platelet count=120×106/L). Peripheral smear revealed leucoerythroblastic blood picture with occasional atypical cells. In view of the above smear picture, bone marrow aspiration (BMA) was done. BMA showed hypercellular particles with diminished trilineage hematopoiesis. Many large atypical pleomorphic cells with high nucleocytoplasmic ratio, basophilic cytoplasm, central to eccentric nucleus with irregular nuclear margin noted. Many such cells showed multinucleation and also nuclear lobation (Figure 1). Few large bizarre cells with abundant basophilic cytoplasm and multilobated nuclei simulating megakaryocytes were also noted. Some of the cells showed peripheral cytoplasmic flare. The possibility of plasma cell myeloma with anaplastic morphology was considered and Immunophenotyping by flowcytometry was done for confirmation. Flowcytometry showed 28.1% neoplastic plasma cells expressing bright CD38 and CD138 along with CD56 (subset), CD28 and cytoplasmic lambda light chain restriction (Figure 2). They were negative for CD19 and CD20. Morphology and Immunophenotypic features were consistent with anaplastic plasma cell myeloma.1 Free light chain assay also confirmed the lambda light chain restriction in neoplastic cells by high lambda (1771mg/L) compared to kappa (10.1mg/L) with ratio of 0.01. The patient was started on cyclophosphamide, bortezomib and dexamethasone, and currently under follow-up.
Anaplastic myeloma is a variant of plasma cell myeloma with an aggressive clinical behavior and poor outcome.1 They can present as a diagnostic dilemma due to their strange morphology. They can mimic as high grade lymphoma or as a non hematopoietic malignancy by morphology. Anaplastic morphology may be seen at initial presentation or later as a progressive transformation of myeloma. Extramedullary infiltration is common.2,3 A constellation of clinical findings along with morphology, biochemical parameters and immunophenotype is mandatory for establishing the correct diagnosis.
Conflicts of interestThe authors declare no conflicts of interest.