With the outbreak of COVID-19 and its containment measures, blood centers faced a huge challenge in balancing blood demand and supply and devising a preparedness plan to withstand the uncertain situation. This study assesses the effect of the COVID-19 pandemic on blood transfusion services and discusses the appropriate mitigation strategies adopted.
MethodsWe analyzed our center's blood transfusion services during the first half-period of the pandemic (Y3) and non-pandemic years 2018(Y1) and 2019(Y2) in two-quarters Q1 (pre-lockdown), from January to March and Q2 (post-lockdown), from April to June. The blood donation variables, the packed red blood cells (PRBCs) demand and the utilization pattern were compared between pandemic (Y3) and non-pandemic years (Y1 and Y2) in each quarter. The mitigation strategy adopted at every step of the transfusion service is highlighted.
ResultsDuring post-lockdown (Q2) of the pandemic year (Y3), the blood donation was majorly by repeat donors (83%) from the in-house site (82.5%). Furthermore, the proportion of outdoor donation, deferral, blood collection, demand and issue demonstrated a significant drop of 50%, 32.6%, 33%, 31.8% and 32.3%, respectively, in comparison to Q2 of the non-pandemic years (Y1 and Y2), with a statistically significant difference for surgical and hemorrhagic indications (p < 0.05). Coping strategies, such as blood donor education and motivation using e-platforms emphasizing eligibility during the pandemic, staggering of donor in-flow, postponement of elective surgeries and donor and staff’ COVID-19 safety assurance, were followed.
ConclusionThe timely adoption of coping strategies played a crucial role in the better handling of shortcomings at our center's blood transfusion services caused by the COVID-19 pandemic.
The World Health Organization (WHO) reported the novel coronavirus (COVID-19) outbreak as a public health emergency of international concern on January 30, 2020 and soon declared it a global pandemic on March 11, 2020.1 Following this, the Central and State governments of India imposed a nationwide lockdown as a precautionary measure to contain the spread of COVID-19.2 This unforeseen situation has dramatically affected healthcare services globally. In particular, this posed a formidable challenge to blood transfusion services in terms of adequate blood inventory management to suffice the blood demand, recruit healthy and non-COVID-19 risk donors and ensure the safety of both blood donors and blood center staff.3,4
In India, the motivation and willingness to donate blood among the general population are low,5,6 let alone in a pandemic situation where considerable uncertainty prevails regarding the safety of blood donation and the risk of transfusion transmission of the infection.7,8 In addition, the restriction put forth in people's movement to contain the disease spread became a hindrance factor for regular voluntary blood donors, even if they wished to donate. As per the National Blood Transfusion Council (NBTC) guidance, blood transfusion centers in India continue to make necessary changes in their policy on donor recruitment, selection and inventory management as the pandemic evolves.9 We planned this study to assess the blood transfusion services, ranging from donor recruitment to blood supply management, during the COVID-19 pandemic at our blood center, and to discuss the confrontation measures adopted to sustain the uninterrupted blood supply in the pandemic period.
MethodsStudy design and settingWe performed a cross-sectional, observational study on the review of blood transfusion services records, such as blood collection and blood demand and issue at our blood center in southern Karnataka during the first half-year period (January to May) of the pandemic year 2020 (Y3) and non- pandemic years 2018 (Y1) and 2019 (Y2).Our blood center is associated with a 2032,-bedded tertiary care hospital catering to the blood need of clinical departments, such as general medicine, surgery, obstetrics and gynecology, pediatrics, orthopedics, dialysis, benign and malignant hematology and emergency and critical care.
Inclusion and exclusion criteriaThis study involved reviewing the records of whole blood donation and the transfusion request received for the crossmatching, typing and screenand issue of packed red blood cells (PRBCs) during the study period. We excluded apheresis donations and other transfusion services, such as therapeutic procedures based on clinician request performed at our center.
Ethical approval:
We obtained ethical approval from our institutional Ethics Committee (Reference no. IEC/334/2020). As the study did not involve any donor or patient identity disclosure risk, the institutional ethical committee waived the requirement for informed consent to review the records.
Data collectionThe data on routine blood transfusion services at our center during the first half-period (January to May) in the COVID-19 pandemic in two-quarters Q1, from January to March, and Q2, from April to June in 2020 (Y3), was retrieved from our department software (Easy Software solutions, Ahmedabad, India). Furthermore, to elicit the actual impact of COVID-19, the concurrent data of the same quarter periods (Q1 and Q2) in the preceding two non-pandemic years of 2018 (Y1) and 2019 (Y2) were also retrieved and compared against the pandemic year. The following data were collected on blood collection, including donor demographics, donation frequency and the blood donation site, whether in-house (blood center premises) or outdoor blood donation drive, and deferral data. In light of the COVID-19 pandemic, blood donor selection and deferral policy during Q2 of the pandemic year were revised as per the interim guidance of the NBTC.9 Accordingly, donors with close contact history with confirmed or suspected COVID-19 patients or with domestic or international travel history were deferred for 28 days and the COVID-19-infected patients were allowed to donate after 28 days of complete recovery. Additionally, the PRBC requests received (crossmatching, typing and screening), crossmatch tests performed and issue of packed red blood cells, including indication-wise utilization during the study period, were observed. Moreover, the COVID-19 mitigation strategies adopted to sustain the blood transfusion services and donor and blood center personnel safety assurance were highlighted.
Statistical analysisThe data analysis was performed using the SPSS version 20 (IBM, Chicago, IL, USA). Descriptive statistics, such as the mean, standard deviation and percentage were used. A one-way ANOVA with a post-hoc Tukey HSD test was used to compare the mean of three years (Y1, Y2, and Y3) and interpret the difference between them. The Student t-test was used to compare both quarter means in the pandemic year (Y3). Categorical variables were analyzed by the Chi-square test (χ2) with the Yate's correction. The p-value < 0.05 was considered statistically significant.
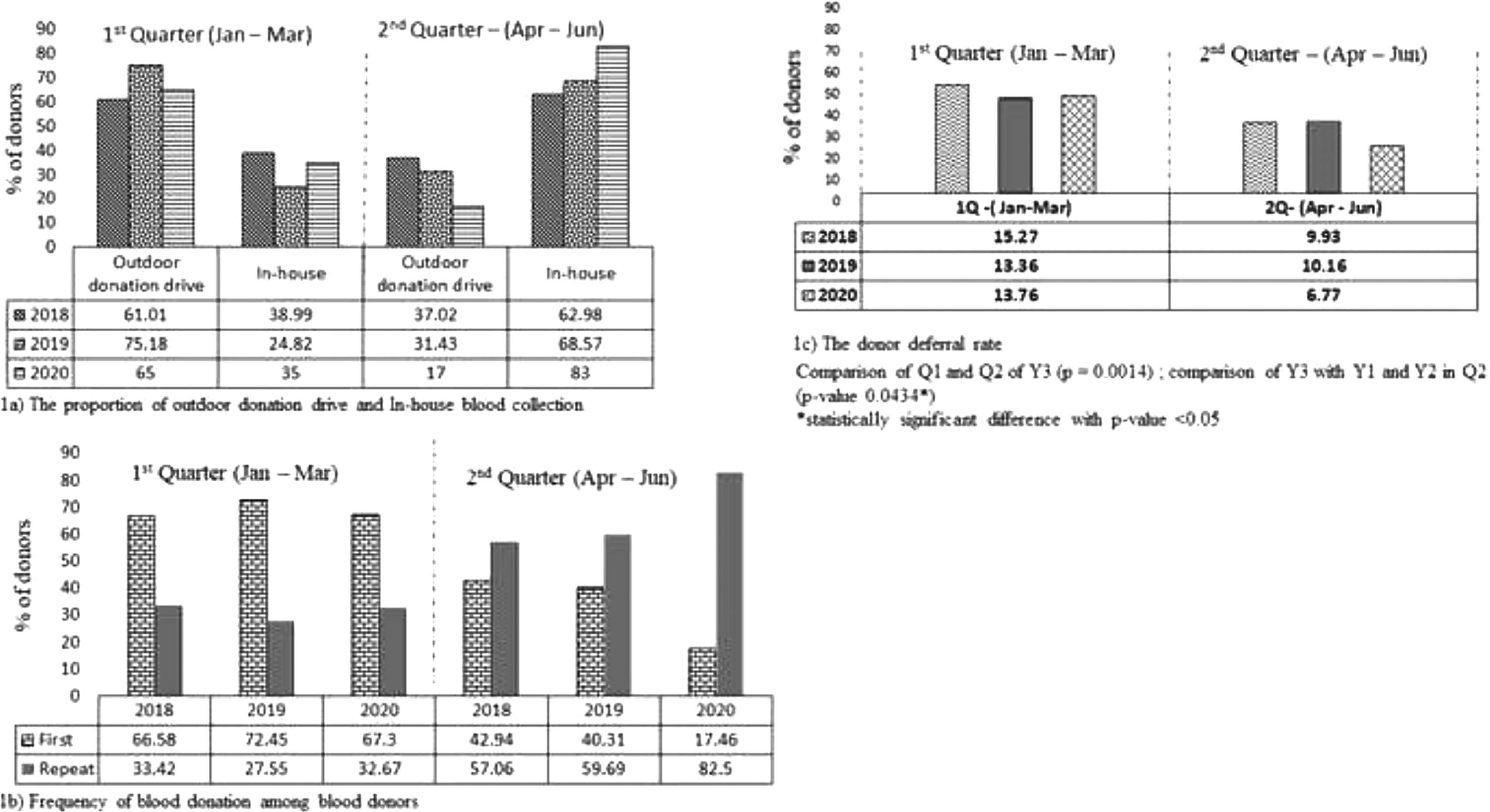
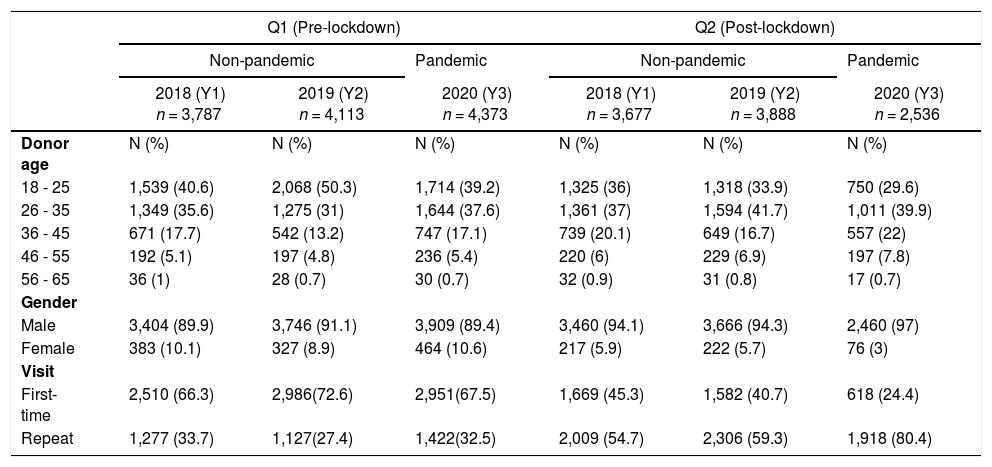
ResultsBlood donationPre-lockdown phase – Q1The donor registrations of the pandemic (Y3) and non-pandemic years (Y1 and Y2) during the pre-lockdown phase account for 5,087, 4,469, and 4,738, respectively, of which the proportion of donors qualified for blood donation were 86.04% (n = 4,377), 84.7% (n = 3,787) and 86.8% (n = 4,113), respectively. As shown in Table 1 and Figure 1, the Q1 phase of both pandemic and non-pandemic years demonstrated a higher proportion of blood donation from male donors, aged 18 to 25 years, and first-time donors from the outdoor blood donation drives, with no statistically significant difference between them. The deferral rate was also found equivalent between the pandemic and non-pandemic years. The common deferral reasons were low hemoglobin, followed by high blood pressure and underweight.
Donor demographic profile.
The donor registration during the Q2 phase of the pandemic year (Y1Y3) was halved (n = 2,730), compared to non-pandemic years Y1 (n = 4,092) and Y2 (n = 4,327), of which the proportion of donors qualified to donate in the pandemic year was 33.05% (n = 2,536) less in comparison to non-pandemic years Y1 (n = 3,688) and Y2 (n = 3,888). As shown in Table 1 and Figure 1, the blood donation in both pandemic and non-pandemic years during the Q2 phase was majorly by male and repeat donors, aged between 26 and 35 years from the in-house site. However, the pandemic year had 26.2% (p > 0.05) and 41.5% (p > 0.05) of increased in-house and repeat donations, but a significant 32.5% (p < 0.05) of less deferral than in non-pandemic years (Y1 and Y2). The deferral reasons are similar to that observed in the pre-lockdown phase, except that 5.4% of the deferrals due to the COVID-19 risk was observed in the pandemic year.
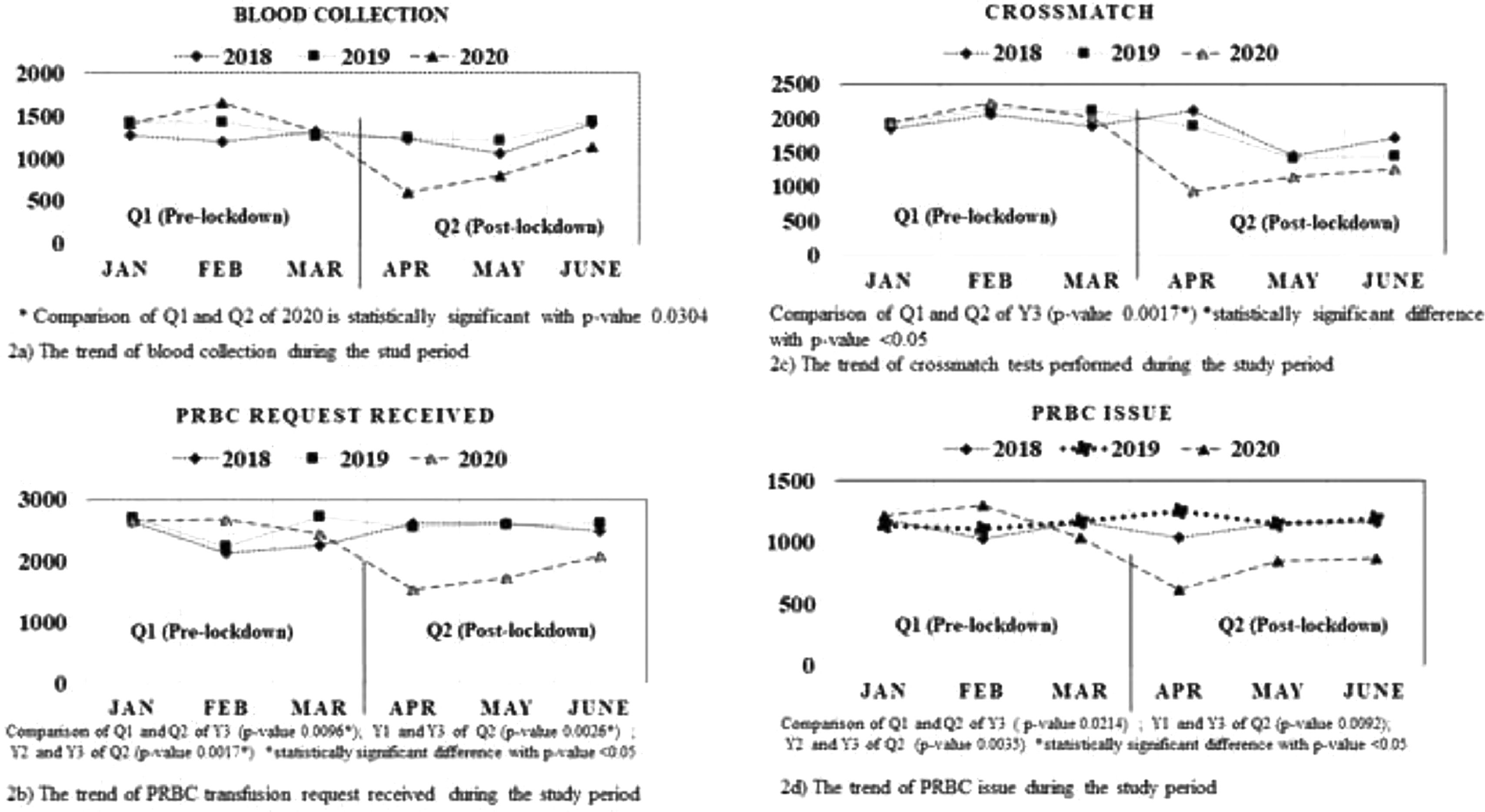
Blood supply managementPre-lockdown phase -Q1The blood supply management in the Q1 phase, as shown in Figure 2, demonstrates the pandemic year (Y3) to have relatively 10.6%, 6%, 4.6% and 4% of increased PRBC collection, demand, crossmatch and issue than the non-pandemic years (Y1 and Y2). However, the difference was not observed to be statistically significant (p > 0.05). Likewise, the PRBC transfusion for indications, such as anemia, hemorrhage, surgery, hemoglobinopathy, dialysis and chemotherapy including massive transfusion, showed no significant difference between the pandemic and non-pandemic years (Figure 3). The massive transfusion protocol (MTP) activation during the pandemic Y3 and non-pandemic years Y1 and Y2 accounted for 29, 32 and 30, respectively, with no statistically significant difference for indications, such as trauma (41.3%), obstetric hemorrhage (37.9%) and upper gastrointestinal (UGI) bleeding (10.3%).
Post-lockdown phase - Q2The pandemic year blood supply management in the Q2 phase, compared to the non-pandemic year, showed 33%, 31.8%, 33.4% and 32.8% of decreased blood collection, demand, crossmatch and issue of PRBC units, respectively, as shown in Figure 2. However, a statistically significant difference, with the p-value < 0.05, was observed only for demand and issue variables between pandemic and non-pandemic years. Similarly, the pandemic year (Y3) showed a significant decrease in PRBC utilization for indications, such as hemorrhage and surgery, with the p-value < 0.05, compared to non-pandemic years (Figure 3). The MTP activation during the Q2 phase accounts for 38, 40 and 19 for non-pandemic years and pandemic year, respectively, accounting for a significant reduction (51.2%; p < 0.05) during the pandemic year.
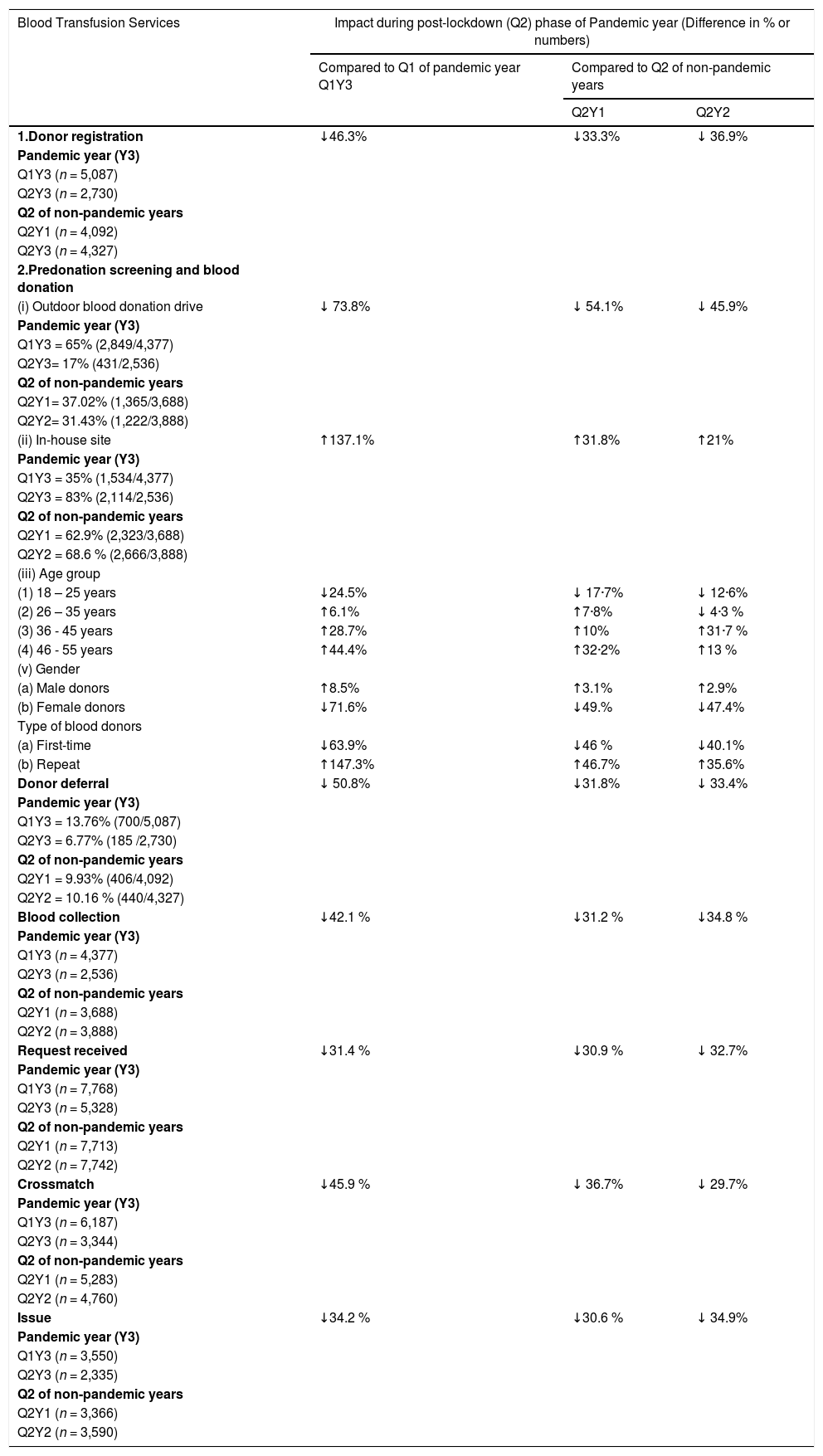
The overall impact of COVID-19 on blood transfusion services of our centre during the post-lockdown phase of the pandemic year is shown in Table 2.
The impact of COVID-19 on blood transfusion services during the post-lockdown phase of the pandemic year.
The summary of the mitigation strategy adopted to sustain regular blood transfusion services at our center is as follows:
Blood donor recruitment- 1.
The circulation of information, education and communication (IEC) materials to donors and blood donation drive organizers addressing the constant blood need, especially for patients on chronic transfusion support, and the COVID-19 symptoms and signs and eligibility criteria for blood donation;
- 2.
The recruitment of potential blood donors among the healthcare personnel of our hospital, and;
- 3.
The reminder calls for eligible blood donors about the completion of their donation interval period
The recommendations to minimize the risk of COVID-19 exposure and ensure blood safety:
- (a)
Blood donors were encouraged to take donor appointment for blood donation to facilitate staggered in-flow of donors;
- (b)
During the lockdown period travel arrangements were made for the donors to reach the blood centre safely;
- (c)
It was mandated to wear face masks and undergo temperature screening and hand sanitization to access the blood center;
- (d)
The donor history questionnaire form was modified to elicit additional history on COVID-19 to promote the selection of the safe and healthy donors;
- (e)
Strict adherence to social distancing and other COVID-19 precautionary measures were followed;
- (f)
Donor couches were placed at a two-meter distance and covered with disposable sheets, which were replaced after every donation;
- (g)
The donors were encouraged to inform the blood center if he or she develops COVID-19 symptoms within 28 days of the donation, and;
- (h)
Donor feedback was obtained on the donation experience.
Donor education was provided on the deferral period of 28 days following recovery or travel history to a COVID-19 infected area and to consider self-deferral by donors with respiratory symptoms or primary contact with COVID-19 infected patients.
Blood supply management- (a)
To minimize the blood demand, the clinicians were requested to follow restrictive transfusion practices and to consider blood alternatives, if applicable, and suggested postponement of elective surgeries;
- (b)
Type and screen rather than crossmatch was adopted for blood requests, if applicable, and;
- (c)
Recommended blood transfusion based on the assessment of risk vs. the benefit to the patient.
- (a)
The blood center was kept functioning with 50% of the staff strength in two shifts per day on rotation every four days;
- (b)
The standing order of consumables based on utilization and inventory was revised, and;
- (c)
The repair and maintenance of equipments were performed by the hospital mechanical and electrical (M&E) department for the temporary period until the travel restrictions were relaxed.
As per the World Blood Donor Day Slogan of 2020,10 “Safe blood saves lives,” recruitment of safe and healthy blood donors amidst the COVID-19 pandemic remains the primary challenge of blood centers and transfusion services globally. Despite the challenges posed, blood centers continue to strive to provide uninterrupted blood supply to meet the ongoing blood need of patients. Moreover, the recommendations by the WHO and other governing and accrediting agencies of blood transfusion services, such as the NBTC, American Association of Blood Banks (AABB) and Centers for Disease Control and Prevention (CDC), paved the way to maintain the safe transfusion chain during the hard times of the pandemic.9,11–13
Blood donationAt our center, the donor registration during the pre-lockdown phase of the pandemic year was found comparable with the non-pandemic years of the same quarter. However, the post-lockdown phase demonstrated 35.13% fewer registrations than the non-pandemic years. A similar reduction in blood donation was observed in the earlier and in the present pandemic periods, with Wang et al. having reported a 67% drop in the whole blood donation in the Zhejiang Province of China, while the Canadian blood services have documented a drop of 30% in the donor attendance rate.14–17 As our blood center is attached to a teaching hospital and surrounded by many educational institutions, a significant proportion of our donor pool comprises the student population and, therefore, blood donation by first-time donors and from outdoor blood donation drives has been a little higher in the Q1 phase in both pandemic and non-pandemic years.
Of note, blood donation at our center during the pandemic year (Y3) was essentially comprised of blood donors aged 26 to 35 years. This is due to non-availability of student donors around March to May of all years for reasons, such as examinations or vacation. In addition, other factors, such as the lock-down, quarantine and restriction in holding outdoor blood donation drives further reduced the donor pool and led us to recruit regular blood donors from our donor registry and motivate healthcare care personnel of our tertiary care hospital. Thus, in-house and repeat donations during the post-lockdown phase of the pandemic year were found to be higher than those in non-pandemic years. Contrary to our findings, few similar studies have reported a higher percentage of first-time donors14 and a significant drop in the in-house site donation during the pandemic year.18 This is probably due to the difference in the epidemiological and geographical factors and donor recruitment strategy as applicable to each centre.
Donor education and awareness played an important role in donor recruitment during the pandemic period.19 Effective communication with blood donors and blood donation drive organizers on donor eligibility and the deferral period, especially regarding COVID-19 through various platforms, including social media, such as WhatsApp and Facebook, proved beneficial at our center in lessening the deferral rate during the post-lockdown phase of the pandemic year (Figure 1). This coping strategy was extensively used as a powerful tool for creating public awareness, the effectiveness of which was well appreciated during the pandemic crisis by the blood centers across the globe.20–23 The common deferral reasons identified in a previous study conducted at our center include the hemoglobin-based deferral followed by high blood pressure.24 However, in the pandemic year post-lockdown phase, a minimal proportion (5.4%) of the deferral was due to the COVID-19 risk. This is probably due to the inclusion of regular blood donors, rather than first-time donors, who are well informed on the blood donation eligibility criteria and, thus, opted for self-deferral.
Blood supply managementThe blood supply management at our center, as shown in Figure 2, demonstrates a minimal rise in blood collection, demand, crossmatch and issue during the pre-lockdown phase of the pandemic year. However, a significant drop in all these variables was noted during April of the pandemic year, followed by a gradual rise from May onwards, reaching towards the baseline of the pre-pandemic years. This observation is found to be in congruence with the implementation and gradual relaxation of the COVID-19 confinement measures. In the literature, the SARS epidemic in 2003 and the present COVID-19 pandemic have shown to cause an imbalance between blood supply and demand, with a significant drop in blood donation.14–21
However, the COVID-19 cope-up measures adopted at our center, such as the temporary suspension of all non-emergency surgical cases, daily monitoring of blood inventory and issue, encouragement of the clinicians to consider blood transfusion only when the benefits outweigh the risk for the patient, promoting type and reserve, rather than crossmatch, to avoid the unnecessary reservation of a blood unit for a particular patient for a prolonged period and the utilization of possible blood alternatives, such as oral or parenteral iron, erythropoiesis-stimulating agents, helped in balancing the demand in face of the blood shortage. Similar strategies adopted by low- and middle-income countries were reported to have a positive effect.18,20
Blood utilizationIn India, as per the National Aids Control Organisation (NACO) report, nutritional anemia (39%), followed by oncological conditions (21.3%) and gastrointestinal bleeds (12.9%), are reported as the common blood requirement needs.25 Similarly, the common indication for the PRBC transfusion at our center, regardless of being pandemic or non-pandemic years, include anemia, surgery and hemorrhage, followed by chemotherapy and others (Figure 3). However, a significant decrease in the PRBC utiliszation for indications, such as hemorrhage and surgery, were noted during the second quarter of the pandemic year, as seen at many blood centers globally.9,2627 This is mainly because of factors, such as the suspension of elective surgeries, decreased the in-flow of patients requiring massive blood transfusion to trauma triage, adoption of thromboelastography (TEG), a real-time global viscoelastic assay-guided transfusion support for bleeding patients and, thereby, to minimize unnecessary transfusion in patients with a normal coagulation status. However, no significant difference in utilization was noted for other indications, such as anemia, hemoglobinopathy and chemotherapy, as most of these patients are dependent on chronic blood transfusion support, with no alternative therapy.
To confront the challenges posed by COVID-19, the mitigation strategy devised at our center consisted of incorporating the COVID-19 recommendation guidelines by various blood authorities and reviewing available literature and peer group experiences shared in the national and international forums, which helped us to overcome the challenges with confidence.3,4,9,12,19 However, these strategies are subjected to revision, as and when the pandemic evolves.
The gist of lessons learned from the present experience in striving for uninterrupted transfusion service is as follows:
- 1.
The maintenance of the donor registry, including the rare donor and the platelet donor registry, is very crucial for a blood center to recruit donors at the time of disaster;
- 2.
Utilisation of social media as a powerful communication medium for donor education and motivation, as well as for the notification of the blood shortage to the public.
- 3.
The blood utilization audits performed at regular intervals enable the understanding of the blood need and the implementation of the necessary changes in the transfusion practice;
- 4.
The reiteration of the rational use of blood components and the adoption of alternate blood strategies are of paramount importance;
- 5.
The strict adherence to the First In, First Out Policy avoids unnecessary wastage of near expiry products;
- 6.
Type and reserve, rather than crossmatch, should be adopted if the blood need is uncertain;
- 7.
Monitoring of reagents, kits and blood bag stock should be performed weekly to identify the near expiry consumables and replace them with a new lot having an extended validity period, and;
- 8.
The utilization of the virtual platform as a source of e-learning and the sharing of peer group experiences improves the transfusion practice.
This study highlights the devastating effects of the COVID-19 pandemic on blood transfusion services at our center, from donor recruitment to inventory and resource management. Furthermore, the lessons learned from our own experience, as well as those of our peer group, played a crucial role in developing coping strategies to sustain continuous blood supply at our center. This experience alerts us to have a preparedness plan to tackle such an unanticipated problem, if faced with one in the future.
CRediT authorship contribution statementDhivya Kandasamy: Data curation, Formal analysis, Writing – original draft. Shamee Shastry: Conceptualization, Writing – review & editing. Deepika Chenna: Formal analysis, Writing – review & editing. Ganesh Mohan: Visualization, Writing – original draft.