Patients with β-thalassemia major (β-TM) are at risk of developing abnormal lipid profiles. Lipid abnormalities, in turn, have a potential role in the pathogenesis of some clinical aspects of thalassemia
ObjectivesTo evaluate lipid levels and atherogenic indices in β-TM patients compared to healthy children and for any association between lipid levels, lipid peroxidation and inflammatory biomarkers
MethodsThis case–control study was carried out on 79 patients with β-TM, aged 6 to 16 years, registered at the Basrah Center for Hereditary Blood Diseases and 85 age- and sex-matched apparently healthy children and adolescents. Complete blood count, serum lipids and ferritin, liver function tests, C-reactive protein (CRP), high-sensitivity CRP (hs-CRP) and serum malondialdehyde (MDA) were evaluated
ResultsPatients with β-TM had significantly lower hemoglobin (Hb), total cholesterol (TC), high-density lipoprotein (HDL), low-density lipoprotein (LDL) and non-high-density lipoprotein (non-HDL) and significantly higher very low-density lipoprotein (VLDL), triglycerides (TGs), LDL/HDL ratio, MDA, hs-CRP, total serum bilirubin (TSB), alanine aminotransferase (ALT) and aspartate aminotransferase (AST) than the control group (p < 0.05). A bivariate analysis revealed that TC has a significant positive association with Hb. The TG has a significant negative association with Hb and a positive association with serum ferritin. Furthermore, MDA, TG, TSB, ALT and AST were significantly positively correlated with serum ferritin (p < 0.05)
ConclusionsAtherogenic dyslipidemia, defined as a high low-density lipoprotein cholesterol (LDL-C/high-density lipoprotein cholesterol (HDL-C) ratio and high TG level, is common among pediatric β-TM patients, it is associated with iron overload and places patients at an increased cardiovascular risk.
β-Thalassemia major (β-TM) is a hereditary anemia resulting from defects in the production of β-globin chains and is one of the most common genetic disorders worldwide.1
Patients with β-TM are at risk of developing iron overload (IOL) in various organs that results from repeated blood transfusions and increased iron absorption by the gastrointestinal tract, which may cause injury particularly to the heart, liver and endocrine glands.1,2
In β-TM, iron overload is associated with increased oxidative stress, lipid peroxidation and liver damage, which account for the lipid abnormalities among these patients.3
Lipids and lipoproteins have a potential role in the pathogenesis of some clinical aspects of thalassemia, including alterations in endocrine function and increased susceptibility to infections and vascular complications such as thromboembolism, which affect β-TM and β-TI patients in a different manner.4 Abnormal lipid profiles have also been correlated with carotid artery intima media thickness and premature atherosclerosis in these patients.5
Many diseases of the liver may affect lipid synthesis and metabolismamong patients with β-TM, including hepatitis C virus (HCV) infection and IOL, iron chelators, mainly deferasirox (DFX) and deferiprone (DFP), are used.6-8
Other causes of lipid abnormalities in thalassemia include higher bone marrow activity with an increased cholesterol requirement for red cell membrane formation.9and lipid peroxidation associated with iron overload.3
Inflammatory biomarker levels, including the C-reactive protein (CRP) and cytokines, are increased in various conditions, including thalassemia. The IOL may play a key role in the release of these markers in β-TM patients.10
High-sensitivity CRP (hs-CRP) and cytokines have been used as biomarkers of inflammation in β-TM. In addition, hs-CRP is useful in thalassemia, as it is shown to be positively associated with the risk of kidney and cardiovascular disease (CVD) in patients with β-TM.11
This case–control study was carried out to evaluate lipid levels and atherogenic indices in patients with β-TM, compared to those of healthy children, to look for any association between lipid levels, lipid peroxidation and inflammatory biomarkers and to assess the association between lipid levels and IOL in β-TM patients.
Subjects and methodsPatientsA case–control study was carried out on patients with β-TM who were registered at the Center for Hereditary Blood Diseases (CHBD) at Basrah Maternity and Children Hospital from November 1, 2014 until the end of April 2015. A total of 79 patients (42 males and 37 females), aged 6 to 16 years, were included in the study.
Full clinical data were obtained, including drug history and associated medical conditions, such as heart failure, diabetes mellitus (DM), hypothyroidism, hyperthyroidism or renal problems.
Patient records were also reviewed as to hepatitis C and B viral infection. No patients were found to have hepatitis B among the studied patients. However, patients with positive hepatitis C antibodies were considered to have hepatitis C infection when a high viral load was confirmed by the polymerase chain reaction (PCR).
Patients excluded from the study were those who had hemoglobinopathies other than β-TM - patients with diabetes mellitus, hypothyroidism, hyperthyroidism or renal failure.4
Control groupThis group included 85 (45 male and 40 female) age- and sex-matched apparently healthy children and adolescents.
Fifty-seven children and adolescents in the control group attended primary health care (PHC) centers for minor health problems, such as cough and cold, tooth extraction or dermatological diseases. In addition, 28 healthy adolescent volunteers from neighbours and relatives were also recruited as controls.
Children and adolescents were excluded in the presence of a family history of hemoglobinopathies or diabetes mellitus, hypothyroidism, hyperthyroidism or renal failure.
Full general and systemic examinations were carried out on all subjects, including vital signs and growth parameters.
Informed consent was obtained from all subjects and/or their families before enrollment in the study, after explaining the purpose of the study and the procedure.
MethodsBlood samples were collected after overnight 12-hour fasting, unless otherwise indicated. Aliquots of blood (1 ml) were collected in EDTA anticoagulant for the hematological study. The rest was left to clot at room temperature (37°C) and centrifuged and the serum was stored at 4°C and used for biochemical analyses within 1 to 2 days, except for MDA, which was performed within 2 to 3 hours.
Hematological studyPatients enrolled in the study were diagnosed with β-TM by High Performance Liquid Chromatography (HPLC), VARIANT™, β-Thalassemia Short ProgramsBio–Rad Laboratories, Hercules, CA, USA.
Complete blood count (CBC): Hemoglobin (g/dl), total white blood cell (WBC) and platelet counts were measured using a SYSMEX KX-21N Automated Hematology Analyzer (Washington or Illinois, United States).
Biochemical analysisSerum lipids profileThe serum lipid profile for patients and adolescent volunteers was determined after 8- to 10- hour fasting:12
For children and adolescents recruited from primary health centers, a non-fasting sample was withdrawn, as fasting may not be necessary for children before lipid screening.13
- 1.
Total cholesterol (TC), triglycerides (TG) and high-density lipoprotein cholesterol (HDL-C) were measured by the enzymatic colorimetric method with a Cobas C111 analyzer (Roche, Germany).
- 2.
Low-density lipoprotein cholesterol (LDL-C) and very low-density lipoprotein (VLDL) were calculated using the Friedewald formula: LDL cholesterol = (TC) - (TG/5) - (HDL cholesterol) and VLDL = TG/5, respectively.
- 3.
Non-HDL was calculated according to the formula: Non-HDL = TC - HDL cholesterol.
- 4.
The atherogenic index (AI): the LDL-C/HDL-C ratio or TC/HDL ratio can be used to assess the AI. In this study, the LDL-C/HDL-C was used because it is highly predictive of major cardiovascular events.14,15
Serum ferritin was assessed using a Mini-Vidas Enzyme-Linked Fluorescent assay provided by Biomerieux SA, France and classified into 3 groups: < 1,000 µg/l, 1,000 to 2,500 µg/l and > 2,500 µg/l.16
Liver function testsTotal serum bilirubin was estimated by a Bilirubinometer (BIL READ) using a special standardized solution put in a capillary tube. The liver enzymes aspartate aminotransferase (AST) and alanine aminotransferase (ALT) were estimated by the fully-automated chemistry analyzer Cobas C111, Japan.
C-reactive protein (CRP)The level was estimated by the rapid latex slide test using a Spectrum Kit, Egypt. The normal level of CRP (< 5 mg/L) was used as a normal value. A value ≥ 5 was regarded as an elevated or abnormal value.
High sensitivity C-reactive protein (hs-CRP)The hs-CRP was measured by the fluorescence immunoassay method according to a kit provided by Boditech Med, Korea.
For children without an overt inflammatory disease, cardiovascular risk assessment cut-offs were recommended as follows: low risk: > 1.0 mg/L, average risk: 1.0 to 3.0 mg/L and high risk: < 3.0 mg/L.17
Estimation of serum malondialdehyde (MDA)The MDA has been identified as the lipid peroxidation product that reacts with thiobarbituric acid to give red species, absorbing at 535 nm.18
Cut-off points for biochemical variablesThe normal values of the biochemical variables were estimated according to values measured for healthy children and adolescents recruited in this study.
All biochemical tests were divided into low values (< 2 SD from the mean), normal values (within the mean ± 2 SD) and high values (> 2 SD from the mean).
Statistical analysisAll statistical analyses were carried out using the Statistical Packages for Social Sciences (SPSS Inc., Chicago, IL, USA) software version 17.0.
Data were expressed by mean ± standard deviation or standard error of the mean, as stated. Comparisons of proportions were performed by cross tab using the chi-square test and Fisher's exact test.
Intraclass differences in parameters between patients and controls, i.e., two means of different samples, were analysed using the independent t-test. Statistical tests with a p-value < 0.05 were considered statistically significant. A bivariate correlation analysis was used to assess the correlation between selected variables and TC and TG levels in patients with β-TM and between IOL and liver profiles, lipid profile and MDA.
ResultsThe total number of children and adolescents enrolled in this study was 164: (79) patients with β-TM and (85) apparently healthy children and adolescents as the control group.
The mean age (± SD) of patients with β-TM was 9.62 ± 3.23 years, while that of the control group was 9.43 ± 2.94 years (p > 0.05).
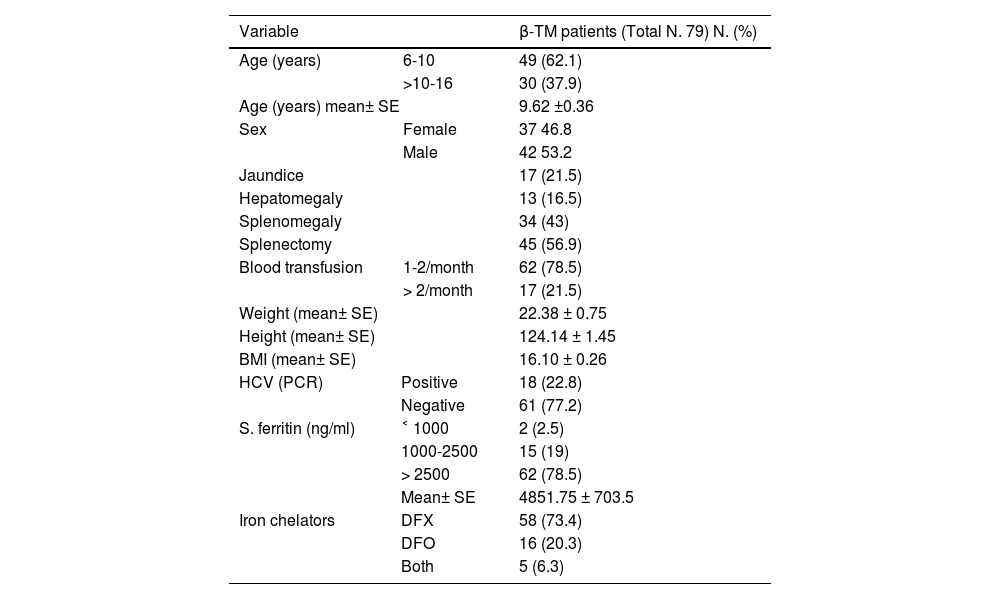
All β-TM patients were on blood transfusion, with 45 (56.9%) of them having been splenectomized. The main clinical findings of patients with β-TM were jaundice in 17 (21.5%), splenomegaly in 34 (43%) and hepatomegaly in 13 (16.5%) (Table 1).
Selected demographic and clinical variables of the studied β-TM patients.
Abbreviations: Body mass index (BMI), hepatitis C virus (HCV), Polymerase chain reaction (PCR), Deferasirox (DFX), Deferoxamine (DFO).
The BMI of β-TM patients was (16.10 ± 2.32), significantly lower than that of the control group (17.35 ± 2.23), p = 0.34.
The mean serum ferritin of β-TM patients was 4,851.75 ± 6,252.37 ng/ml, with 62 (78.5%) having serum ferritin levels above 2,500 ng/ml.
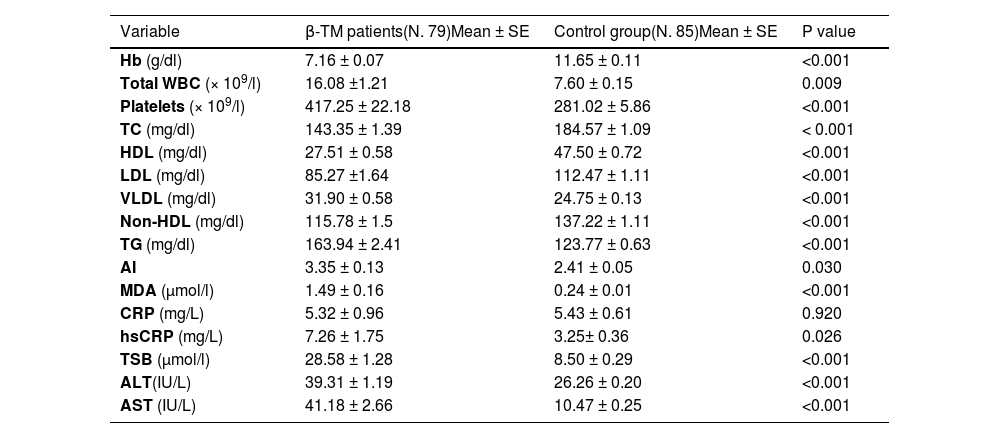
Patients with β-TM had significantly lower Hb, serum TC, HDL, LDL and non-HDL and significantly higher WBC and platelet counts, serum VLDL, TG, LDL/HDL ratio, MDA, hsCRP, TSB, ALT and AST than the control group (p < 0.05, Table 2).
Selected hematological and biochemical variables of β-TM patients and the control group.
Independent t-test was used.
Abbreviations: hemoglobin (Hb), Total cholesterol (TC), high-density lipoprotein cholesterol (HDL-C), low-density lipoprotein cholesterol (LDL-C), very low-density lipoprotein (VLDL), triglycerides (TG), atherogenic index (AI), C-reactive protein (CRP), Malondialdehyde (MDA), high sensitivity C-Reactive Protein (hsCRP), total serum bilirubin (TSB), aspartate aminotransferase (AST), alanine aminotransferase (ALT).
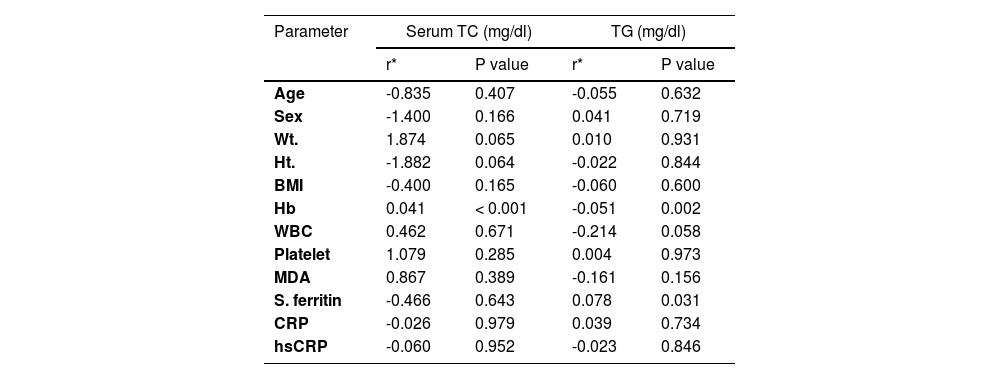
A bivariate analysis of different factors and biochemical tests that could be associated with lipid profiles among patients with β-TM was assessed and revealed that the TC has a significant positive association with the Hb. For the TG, a significant negative association with the Hb and a positive association with the serum ferritin were demonstrated (Table 3). Furthermore, the MDA, TG, TSB, ALT and AST were significantly positively correlated with the serum ferritin, while the VLDL, in addition to the TC, were significantly positively correlated with the Hb (p < 0.05, Table 4).
Correlation of selected variables with TC and TG levels in patients with β-TM.
| Parameter | Serum TC (mg/dl) | TG (mg/dl) | ||
|---|---|---|---|---|
| r* | P value | r* | P value | |
| Age | -0.835 | 0.407 | -0.055 | 0.632 |
| Sex | -1.400 | 0.166 | 0.041 | 0.719 |
| Wt. | 1.874 | 0.065 | 0.010 | 0.931 |
| Ht. | -1.882 | 0.064 | -0.022 | 0.844 |
| BMI | -0.400 | 0.165 | -0.060 | 0.600 |
| Hb | 0.041 | < 0.001 | -0.051 | 0.002 |
| WBC | 0.462 | 0.671 | -0.214 | 0.058 |
| Platelet | 1.079 | 0.285 | 0.004 | 0.973 |
| MDA | 0.867 | 0.389 | -0.161 | 0.156 |
| S. ferritin | -0.466 | 0.643 | 0.078 | 0.031 |
| CRP | -0.026 | 0.979 | 0.039 | 0.734 |
| hsCRP | -0.060 | 0.952 | -0.023 | 0.846 |
Abbreviations: hemoglobin (Hb), Total cholesterol (TC), triglycerides (TG), weight (Wt), height (HT), body mass index (BMI), C-reactive protein (CRP), Malondialdehyde (MDA), high sensitivity C-Reactive Protein (hsCRP).
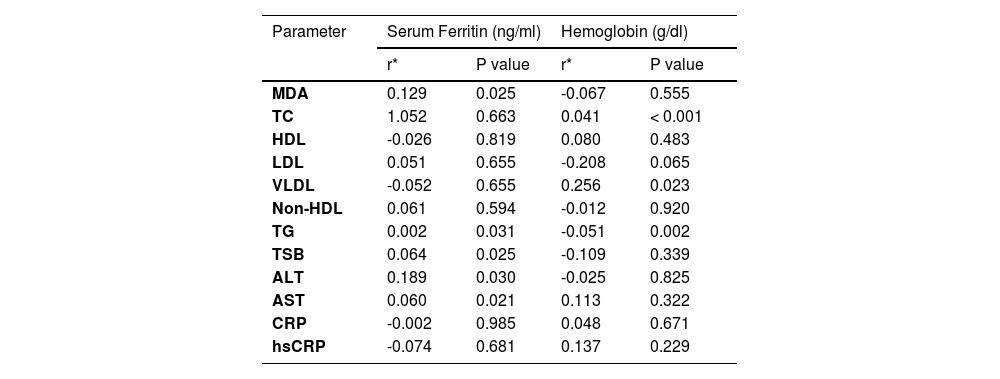
Correlation of lipids and selected biochemical markers with ferritin and hemoglobin in patients with β-TM.
| Parameter | Serum Ferritin (ng/ml) | Hemoglobin (g/dl) | ||
|---|---|---|---|---|
| r* | P value | r* | P value | |
| MDA | 0.129 | 0.025 | -0.067 | 0.555 |
| TC | 1.052 | 0.663 | 0.041 | < 0.001 |
| HDL | -0.026 | 0.819 | 0.080 | 0.483 |
| LDL | 0.051 | 0.655 | -0.208 | 0.065 |
| VLDL | -0.052 | 0.655 | 0.256 | 0.023 |
| Non-HDL | 0.061 | 0.594 | -0.012 | 0.920 |
| TG | 0.002 | 0.031 | -0.051 | 0.002 |
| TSB | 0.064 | 0.025 | -0.109 | 0.339 |
| ALT | 0.189 | 0.030 | -0.025 | 0.825 |
| AST | 0.060 | 0.021 | 0.113 | 0.322 |
| CRP | -0.002 | 0.985 | 0.048 | 0.671 |
| hsCRP | -0.074 | 0.681 | 0.137 | 0.229 |
Abbreviations: Total cholesterol (TC), high-density lipoprotein cholesterol (HDL-C), low-density lipoprotein cholesterol (LDL-C), very low-density lipoprotein (VLDL), triglycerides (TG), C-reactive protein (CRP), Malondialdehyde (MDA), high sensitivity C-Reactive Protein (hsCRP), total serum bilirubin (TSB), aspartate aminotransferase (AST), alanine aminotransferase (ALT).
This study discussed the blood lipid levels of children and adolescents with β-TM in Basrah. The study observed low total serum cholesterol, HDL cholesterol and LDL cholesterol with an elevation of TG and AI in β-TM patients, compared to control subjects. It also revealed a positive correlation between the TG, MDA and serum ferritin.
Abnormal blood lipid levels, such as the TC and other lipids and lipoproteins, adversely affect atherosclerotic diseases. The low total levels of serum cholesterol, HDL cholesterol and LDL cholesterol, with elevated TGs in β-TM patients, compared to control subjects, agree with the findings of other studies regarding the altered serum lipid pattern in β-TM patients, as in Ragab et al. in Egypt19 and Bordbar et al. in Iran.20 These alterations are likely due to diminished hepatic biosynthesis due to anemia and IOL and accelerated erythropoiesis, with excess uptake of cholesterol by macrophages of the reticuloendothelial system, while reduced extrahepatic lipolytic activity could account for the rise in the circulating TG.5
We also found that the TC was positively correlated with hemoglobin levels. Daswani et al., also reported a similar finding.21 This result can be explained by the presence of enhanced cholesterol consumption required for cell membrane formation and the presence of a hyperplastic and overactive reticuloendothelial system.22
The AI, as assessed by the LDL-C/HDL-C ratio, was significantly higher in patients than in the control group. Dyslipidemia and high AI can be attributed to chronic hemolysis, that causes a dysregulated arginine metabolism, with a low arginine/ornithine ratio due to the release of arginase enzyme from RBCs, coupled with the liberation of cell-free hemoglobin. This hemolysis will limit arginine availability to nitric oxide synthase and lead to vascular dysfunction by disturbing the bioavailability of nitric oxide (NO).5
The serum TG had a significant negative correlation with Hb among thalassemic children. This correlation can be attributed to anemia, placing patients at risk for decreased extrahepatic lipolytic activity, resulting in high serum TG.19 Additionally, the TG has a positive correlation with serum ferritin in β-TM children, which agrees with that reported by Sherief et al.5and Ragab et al.19, both in Egypt. These results might support the hypothesis that both serum iron and TG are involved in the pathogenesis of LDL-C oxidation.23
Peroxidative damage to lipids is indicated by an increase in serum MDA and a decreased antioxidant defense mechanism, which play an important role in the pathogenesis of β-TM.24 Elevated serum MDA in the β-TM group, compared to the control group, was reported in the current study. This result agrees with that found by Patne et al. in India24 and Gunarsih et al. in Indonesia.25 The elevated MDA demonstrated that the LDL-C from β-TM patients is more prone to peroxide formation. Therefore, organ damage (in particular the liver) and the relative increased risk of cardiovascular disease could be linked to the greater oxidative stress and oxidation in the LDL-C, even in β-TM patients with low TC and LDL-C concentrations.3
C-reactive proteins and cytokines were used as biomarkers of inflammation in β-TM in the current study. The hs-CRP was significantly elevated in β-TM patients, compared to the control group. This elevation agrees with that found by other researchers in Iraq.10,26 However, our finding is in contrast to that reported by Ehteram et al., who reported that the levels of hs-CRP were not significantly different between patients and the control group.11 It was found in the present study that approximately half of the patients were in the high-risk group.
The hs-CRP levels may indirectly reflect baseline cardiovascular fitness because regular physical activity lowers the hs-CRP.27 The protective association of the HDL-C with coronary heart disease (CHD) and the CVD is diminished when hs-CRP levels are <3 mg/L. Inflammation might negatively modify the HDL, indicating that in the presence of systemic inflammation, HDL particles contain less cholesteryl ester and become larger and more enriched with free cholesterol, TGs and free fatty acids (FFAs). Thus, the HDL becomes less antioxidative and less efficient at removing cholesterol from cells. Others have also reported dysfunctional HDL, demonstrating impaired reverse cholesterol transport.28
The β-Thalassemia major patients had significantly elevated liver enzymes ALT and AST, compared with the control group. This elevation agrees with other studies by Sherief et al.5 and Ragab et al.19. The elevated liver enzymes can be attributed to iron deposition and infection by hepatitis B and C. Elevated serum transaminases in patients indicate massive cell membrane damage in tissues, especially in the liver. Both the IOL and oxidative stress gradually damage tissues, mainly the liver, pancreas and myocardium. In addition, liver cell damage contributes to changes in plasma lipid patterns and the lipoprotein composition in β-TM patients.29
Regular blood transfusions and ICT have substantially improved the quality of life and extended the lifespan of these patients. However, it results in the IOL and its complications. The serum ferritin is a convenient measure of the iron status in patients with β-TM, especially in countries where other methods are not available, as in Iraq.
In the current study, the average serum ferritin was considerably higher than its peak value (1,000 µg/L). Iron plays a catalytic role in initiating free reactive oxygen species (ROS), presumably through iron-initiated Fenton chemistry. The resulting ROS can damage cellular lipids, nucleic acids, proteins and carbohydrates.30 The increased relative risk of CVD and organ damage (particularly in the liver) could be linked to the greater oxidative stress and oxidation in the LDL-C, even in patients with lower TC and LDL-C concentrations. The IOL causes increased oxidative stress, a deleterious factor leading to insulin resistance and increased VLDL production. Increased VLDL production and impaired VLDL lipolysis link a high TG level with a low HDL-C concentration.3
One limitation of the study is that it was a cross-sectional study, rather than a longitudinal study, which would have allowed us to follow serum lipids over time. Another limitation is that we used serum ferritin only as an indicator of iron overload, as it is the only available tool in our country
ConclusionsAtherogenic dyslipidemia, defined as a high LDL-C/HDL-C ratio and high TG level, is common among pediatric patients with β-TM and is associated with the hemoglobin level and iron overload. Early detection of these changes is important to prevent the increased cardiovascular risk associated with atherogenic dyslipidemia in the future.
AuthorshipHK, MK and LA designed and planned the study. HK collected the data. All authors contributed to the analysis and writing of the manuscript and all have read and approved the final manuscript.
FundingNone.
We would like to thank Dr. Maysaa B. Al-Rudainee, Family Medicine Specialist and Dr. Ammar Ali Hussain (Pediatrician) for their great assistance in conducting the statistical analysis of data.