Type 2 diabetes mellitus, characterized by insulin resistance, corresponds to approximately 90% of cases of diabetes worldwide. Hyperglycemia in diabetes contributes to hyperfibrinogenemia and activates the coagulation cascade thereby producing atherothrombotic events.
ObjectivesThis study was designed to evaluate the coagulation profile (activated partial thromboplastin time, prothrombin time and fibrinogen) in Type 2 diabetes and to analyze correlations between body mass index, fasting blood glucose, glycated hemoglobin and duration of diabetes with coagulation parameters.
MethodsThis study included 60 type 2 diabetics and 30 controls. Diabetic patients were grouped in two sets based on the presence or absence of microvascular complications. The demographic profile and clinical details were recorded. Fasting blood glucose, glycated hemoglobin, coagulation parameters such as prothrombin time, activated partial thromboplastin time and fibrinogen along with other biochemical parameters were investigated.
ResultsThere were statistically significant differences in the coagulation parameters between the two groups of diabetics (with and without complications). The present study also found significant correlations between age and the duration of diabetes with and without complications and coagulation parameters such as the activated partial thromboplastin time, which was found to be significantly lower, and fibrinogen, which was found to be significantly higher in subjects with complications compared to subjects without complications.
ConclusionClinical tests for prothrombin time, activated partial thromboplastin time and fibrinogen are relatively inexpensive and readily available. The present study shows that shortened prothrombin time, activated partial thromboplastin time and increased fibrinogen levels might be useful hemostatic markers in diabetic patients, especially in those at high-risk for thrombotic complications.
Diabetes mellitus (DM) is a major global health problem. Type 2 DM, characterized by insulin resistance, corresponds to approximately 90% of the cases of diabetes worldwide.1 Patients with DM have a high risk of atherothrombotic events with 80% of DM patients dying a thrombotic death and 75% of these deaths being due to cardiovascular complications.2 Measurement of prothrombin time (PT), activated partial thromboplastin time (APTT), bleeding time and clotting factor concentration are usually carried out in patients with a suspected abnormal coagulation. Plasma fibrinogen is also an important component of the coagulation cascade and a major determinant of blood viscosity and blood flow. It has also been reported that fibrinogen is a strong cardiovascular risk factor in the general population and increased plasma levels of fibrinogen have been reported in type 2 DM patients.3 The current study focuses on the importance of routine determination of PT and APTT along with fibrinogen levels in order to assess the impairment of the coagulation cascade in DM and to evaluate the association in DM patients with complications and hypercoagulability.
MethodsThis case control study was conducted in the Department of Pathology of the Employees State Insurance Corporation (ESIC) Medical College and Hospital, Faridabad, Haryana after approval from the Institutional Ethics Committee. The research was performed over a period of three months (July to Sept 2017). It included 60 type 2 DM patients and 30 apparently healthy individuals (controls) matched for age and body mass index (BMI). Diabetic patients were grouped in two sets as 30 patients without complications and 30 patients with some type of microvascular complication such as retinopathy, nephropathy or neuropathy based on ophthalmoscopy examination, renal function tests and nerve conduction studies, respectively.
The glycated hemoglobin (HbA1c) level of all patients was estimated using an automated analyzer (Randox Daytona). Furthermore, based on the HbA1c levels, diabetic patients were also grouped as DM with HbA1c≤7% and DM with HbA1c>7%. The inclusion criteria were non-insulin dependent type 2 DM patients, on treatment, attending medical clinics and ready to give consent. The demographic profile (weight and height, age, and sex) and clinical details including duration of diabetes, family history, hypertension, drug history and associated complications or comorbidities were recorded. BMI as an index to estimate the extent of obesity was calculated by the formula body weight (kg) divided by the square of the height (m).
The exclusion criteria considered were patients with a history of predisposition to hypercoagulability, including thrombocytosis, history of venous thromboembolism, known inherited coagulation disorders, cancer, pregnancy, recent surgery, hyperthyroidism and patients who were receiving standard anticoagulant treatment with either coumarin derivatives or heparins at the time of admission. Also excluded were patients with type 1 diabetes and a BMI equal to or greater than 28kg/m2.
Venous blood samples (12–15mL) were collected in three vacutainers. Ethylenediaminetetraacetic acid (EDTA) vacutainers were used to investigate HbA1c in a D10 analyzer by high performance liquid chromatography, fluoride vacutainers were used for fasting and post-prandial blood sugar levels and citrated blood was used for APTT, PT and fibrinogen measurement with coagulation investigated in a fully automated coagulometer (Stago STA Compact Max). Plain vacutainers were employed for the liver function test (LFT), kidney function test (KFT) and calcium/phosphorous/alkaline phosphatase (Ca/Phos/ALP) using the colorimetric method in a fully automated biochemistry analyzer. Samples were collected in the morning for fasting blood sugar and two hours later (post-prandial). Samples were collected at the same time for all other tests.
Statistical analysisAll data were compiled and analysis was achieved using the Statistical Package for Social Sciences (SPSS) version 17 software; student t-test, one-way analysis of variance (ANOVA) along with Mann–Whitney U tests were used for the analyses. A p-value of <0.05 was considered significant. The results are presented as means±standard deviation (SD) and percentages.
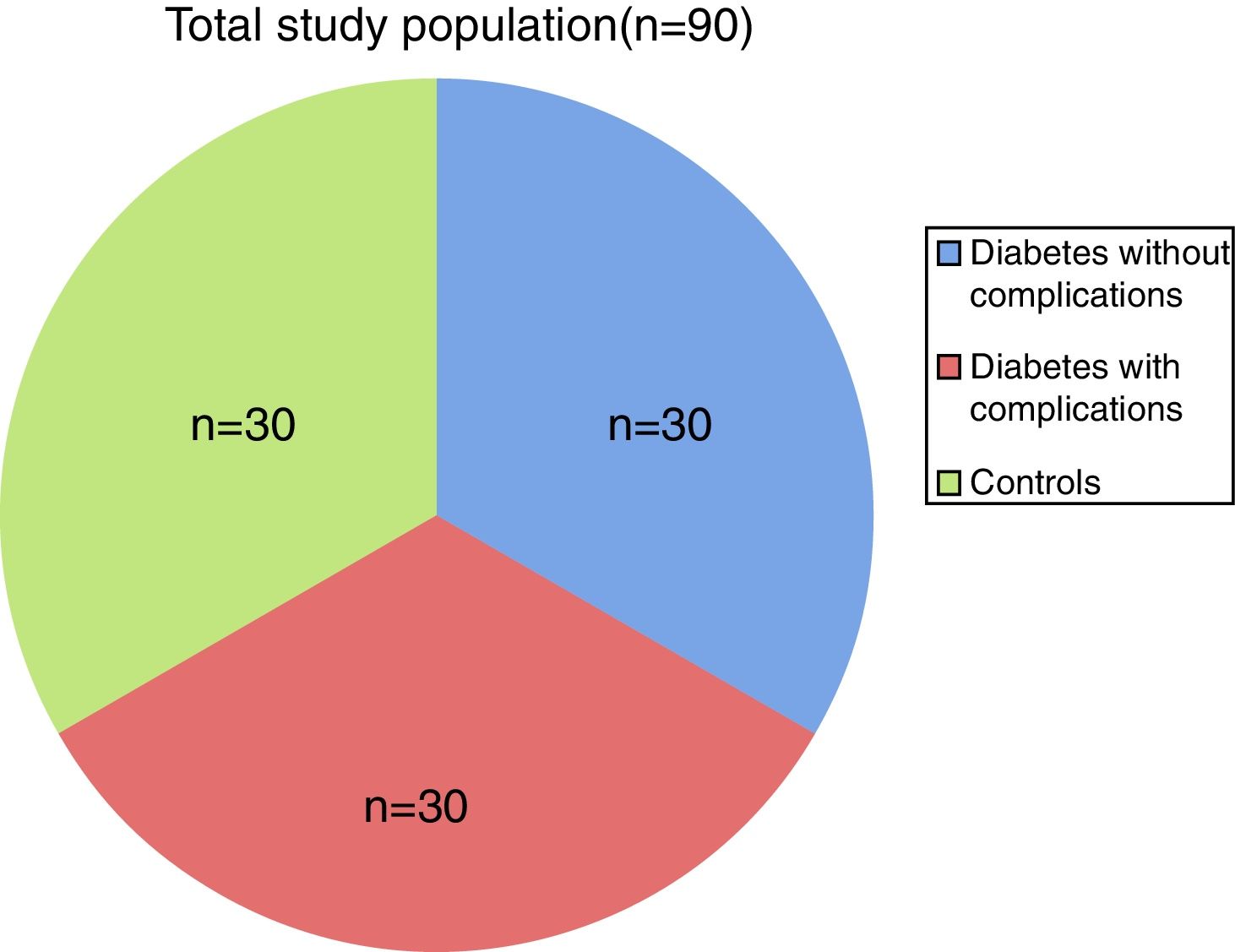
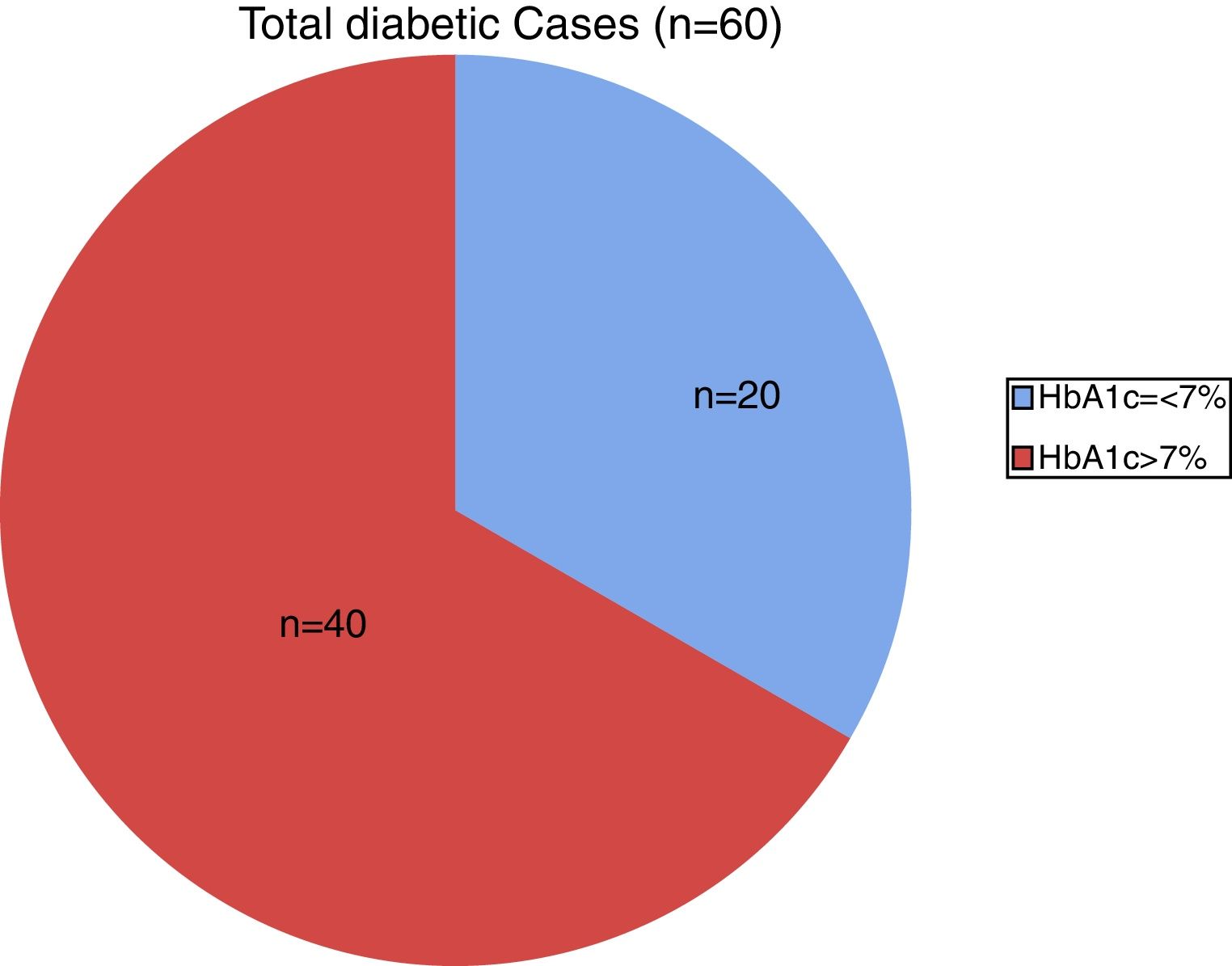
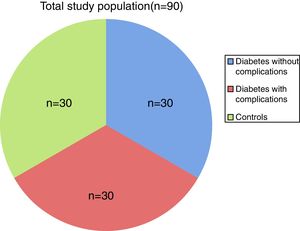
ResultsThis study examined the hemostatic profile of diabetic patients. The study population included 60 diabetic patients (cases) divided into two groups: Group I – diabetes without complications (n=30) and Group II – diabetes with complications (n=30) and a control group was formed of 30 apparently normal individuals as shown in Figure 1. Group I (diabetics without complications) was comprised of 16 females and 14 males (ratio: 1.14:1). The mean age was 50.87±9.75 (range 33–70 years) with most of the patients in the 40- to 50-year age group (n=15; 50%), followed by 51–60 years (n=7; 11%). The study showed mean duration of diabetes as 2.5 years.
Group II (diabetics with complications) was comprised of 15 females and 15 males (ratio: 1:1). The mean age was 55.63±7.49 (range: 35–70 years) with most of the patients in the 50- to 60-year age group (n=20; 66.6%). The mean duration of diabetes was eight years. Twenty-three patients had retinopathy, 13 had neuropathy, ten had microangiopathy and eight had nephropathy with many patients suffering from more than one complication.
On comparing the age and duration of diabetes in respect to APTT, a statistically significant correlation was found (p-value <0.00001). However, there was no significant association with the BMI.
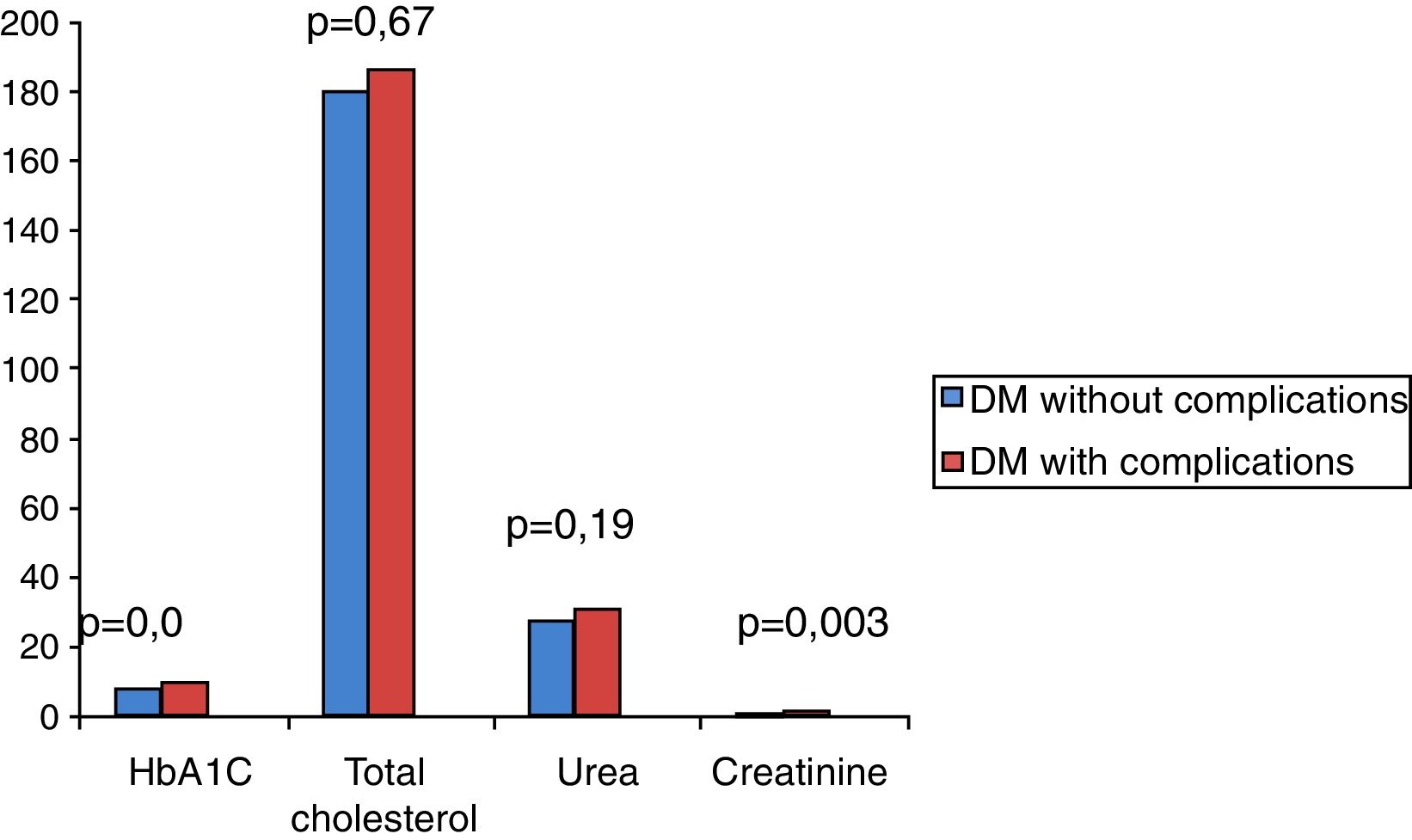
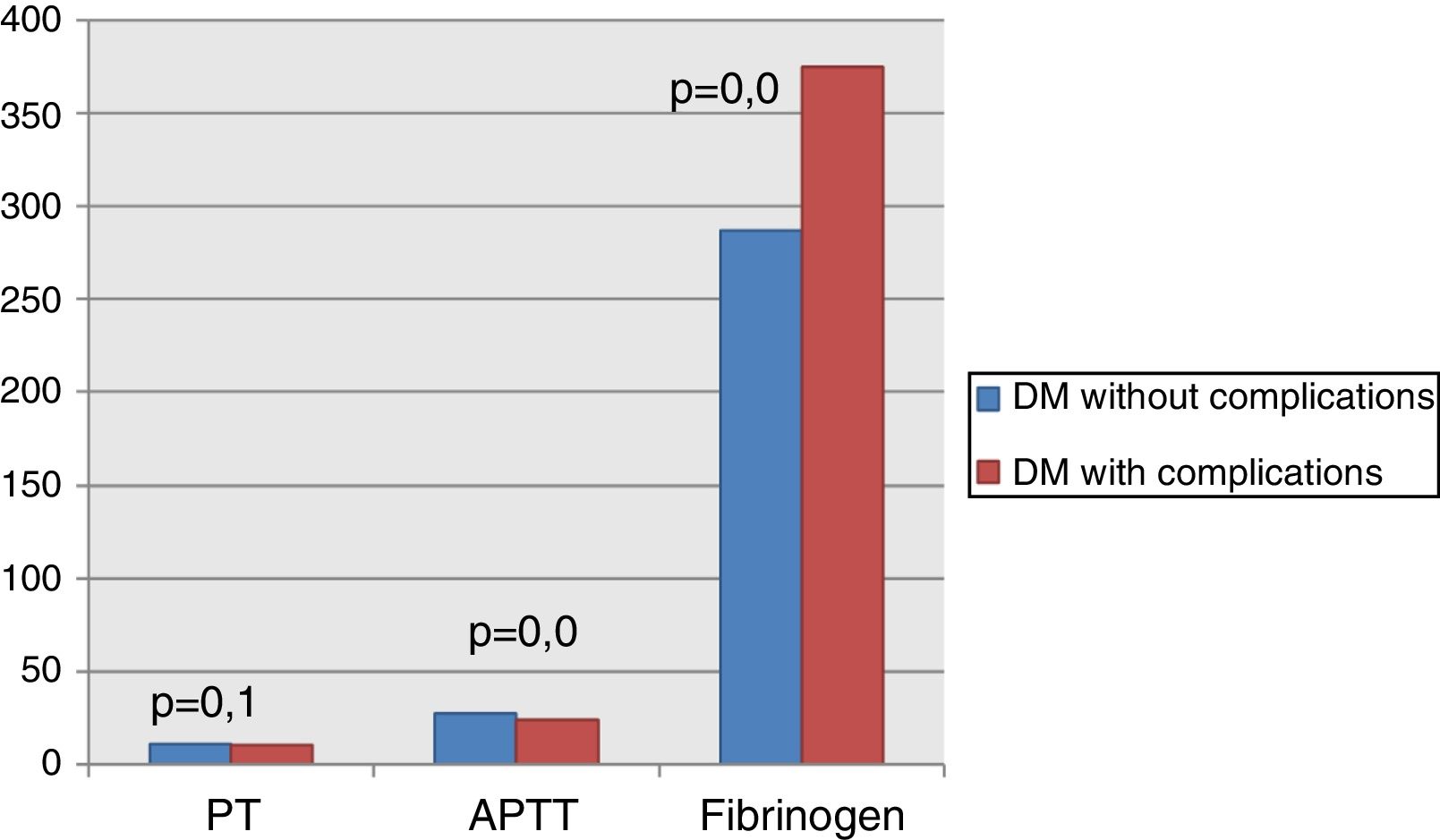
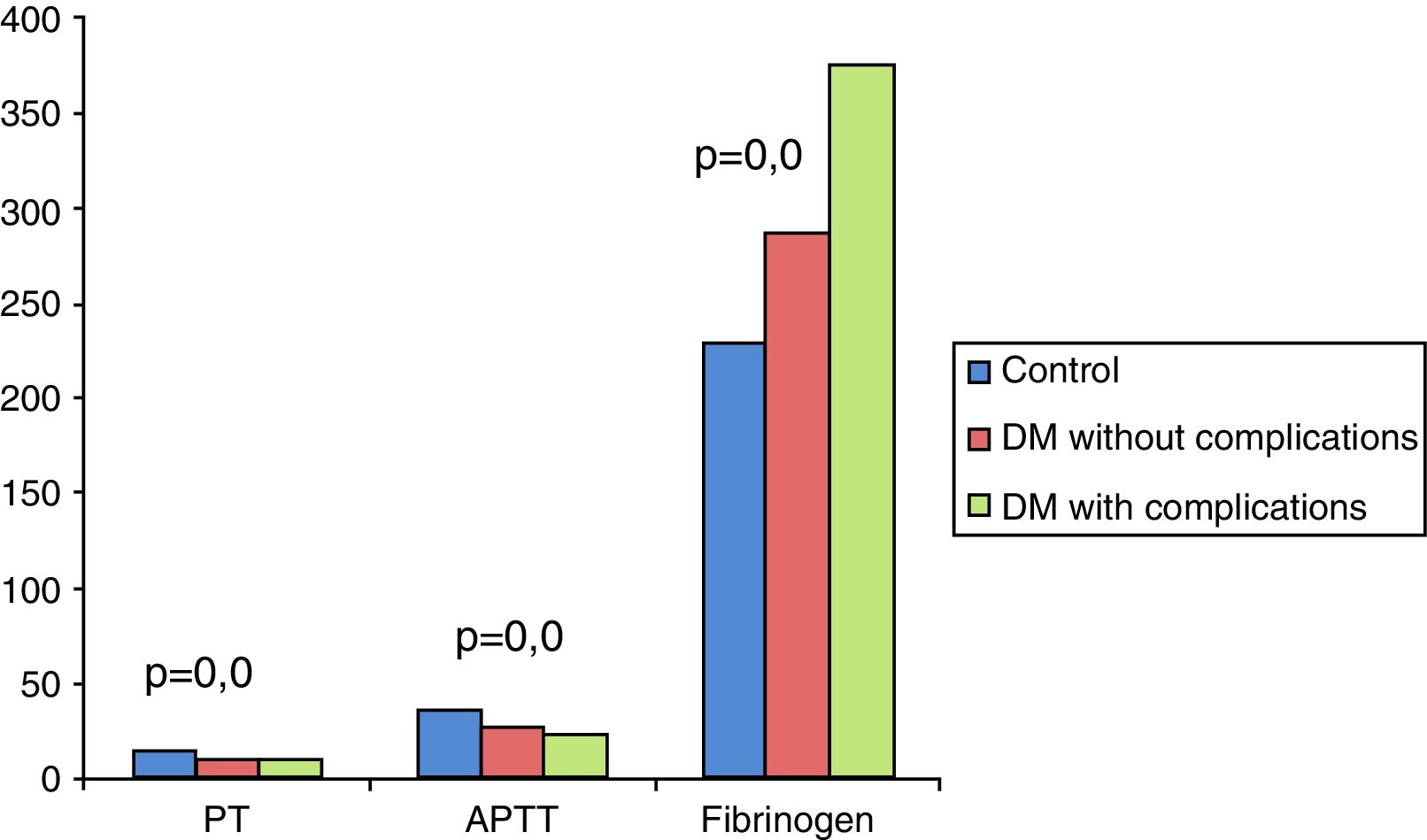
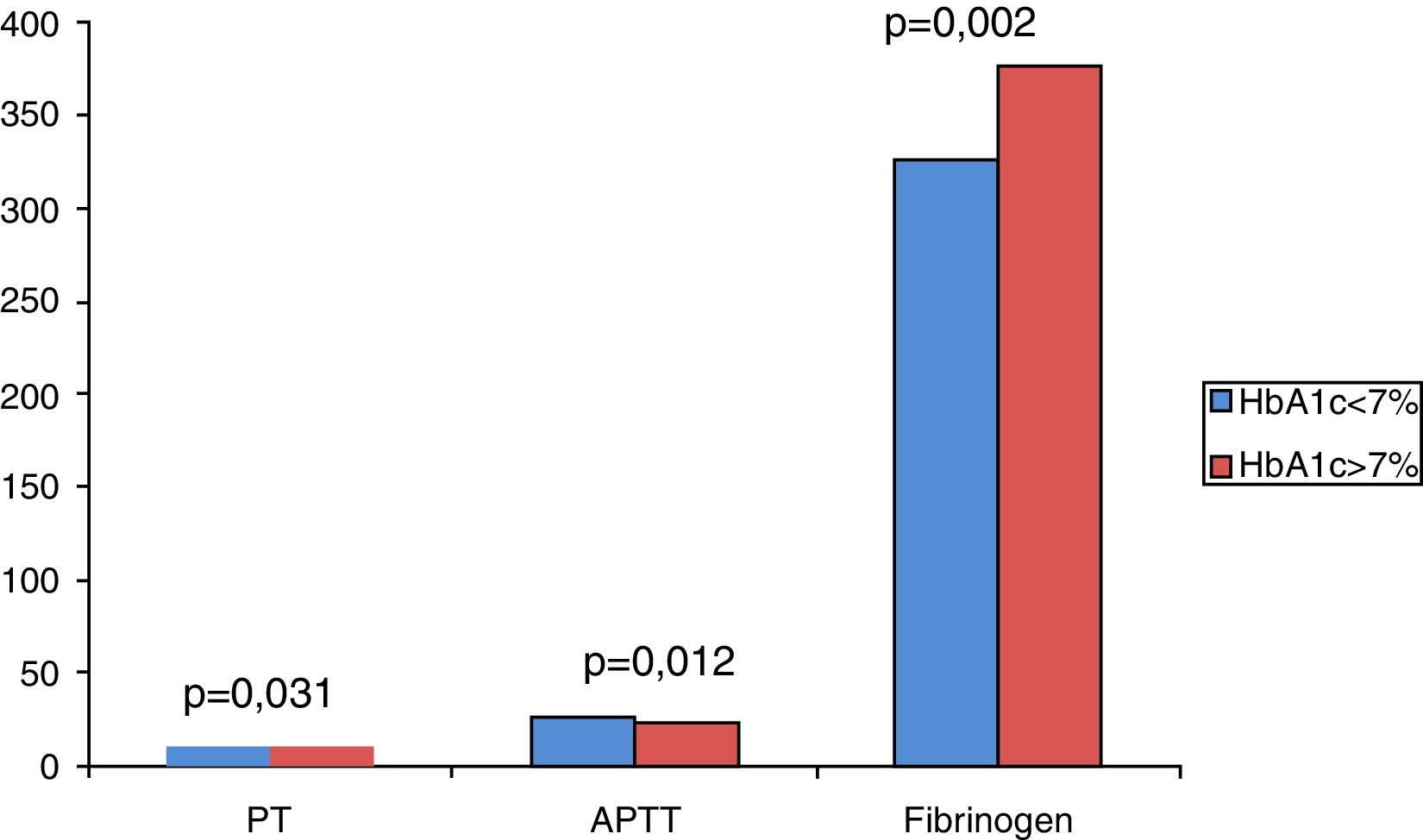
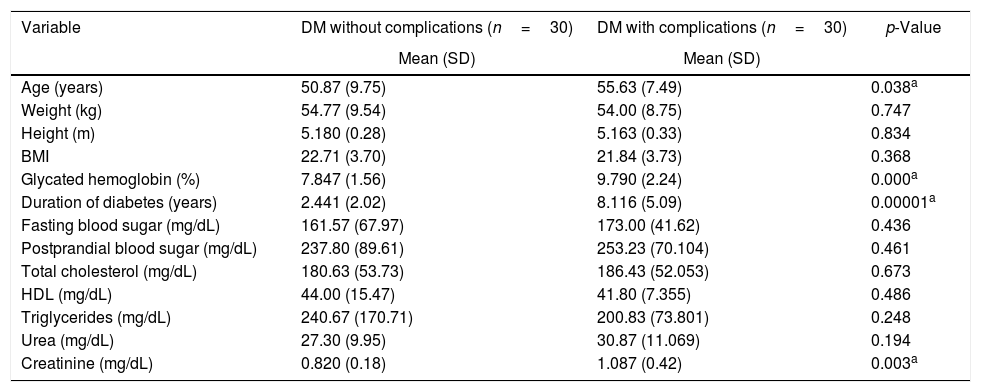
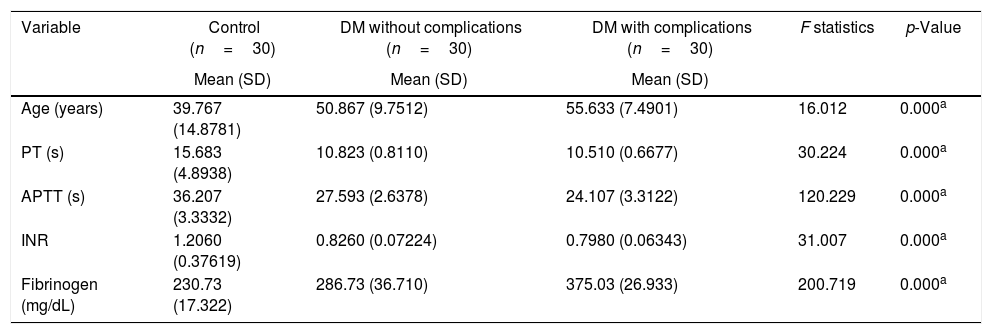
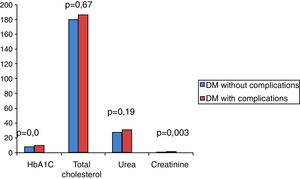
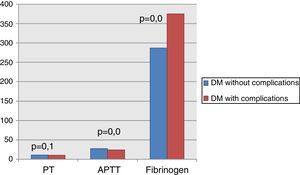
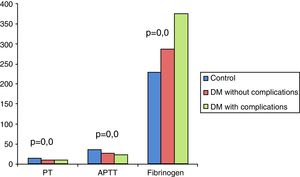
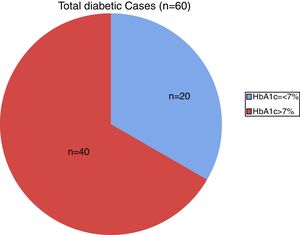
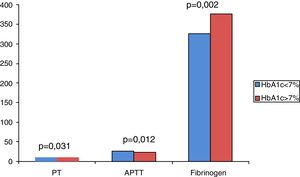
On analyzing the clinical and biochemical parameters using the t-test, it was found that variables such as age, duration of diabetes, HbA1c and creatinine were statistically significant between diabetics with and without complications (Table 1). Diabetics with complications had a significantly higher mean age compared to those without complications (55.63±7.49 vs. 50.87±9.75; p-value=0.038). The mean duration of diabetes (in years) in patients without complications was lower compared to those with complications (2.44±2.03 vs. 8.12±5.09). HbA1c and creatinine were found to be significantly higher in diabetics with complications compared to diabetic patients without complications. However, there were no significant differences in respect to sex, BMI and other biochemical parameters between both the groups (Figure 2). There was a statistically significant difference in coagulation parameters between the two groups of diabetics (Table 2). APTT was found to be significantly lower (p-value=0.000) and fibrinogen was found to be significantly higher (p-value=0.000) in subjects with complications compared to subjects without complications. However, PT did not show any significant difference between the groups (Figure 3). On applying the one-way ANOVA test to compare the three groups, statistically significant differences in age and all the coagulation parameters (PT, APTT and fibrinogen) were found between diabetics with complications, those without complications and the Control Group (Table 3 and Figure 4). Moreover, the diabetic patients (n=60) were reclassified based on HbA1c levels: DM with HbA1c≤7% (n=20) and DM with HbA1c>7% (n=40) as shown in Figure 5. On applying the Mann–Whitney U test to these two groups, fasting and postprandial blood sugar levels were found to be significantly higher among diabetic patients with HbA1c>7% compared to those with HbA1c≤7%. However, the other clinical and biochemical parameters did not show any statistical differences (Table 4). Among coagulation parameters, PT and APTT were found to be significantly lower and fibrinogen was found to be significantly higher in patients with HbA1c>7% compared to patients with HbA1c≤7% (Table 5 and Figure 6).
Comparison of clinical and biochemical parameters between diabetic patients with and without complications.
| Variable | DM without complications (n=30) | DM with complications (n=30) | p-Value |
|---|---|---|---|
| Mean (SD) | Mean (SD) | ||
| Age (years) | 50.87 (9.75) | 55.63 (7.49) | 0.038a |
| Weight (kg) | 54.77 (9.54) | 54.00 (8.75) | 0.747 |
| Height (m) | 5.180 (0.28) | 5.163 (0.33) | 0.834 |
| BMI | 22.71 (3.70) | 21.84 (3.73) | 0.368 |
| Glycated hemoglobin (%) | 7.847 (1.56) | 9.790 (2.24) | 0.000a |
| Duration of diabetes (years) | 2.441 (2.02) | 8.116 (5.09) | 0.00001a |
| Fasting blood sugar (mg/dL) | 161.57 (67.97) | 173.00 (41.62) | 0.436 |
| Postprandial blood sugar (mg/dL) | 237.80 (89.61) | 253.23 (70.104) | 0.461 |
| Total cholesterol (mg/dL) | 180.63 (53.73) | 186.43 (52.053) | 0.673 |
| HDL (mg/dL) | 44.00 (15.47) | 41.80 (7.355) | 0.486 |
| Triglycerides (mg/dL) | 240.67 (170.71) | 200.83 (73.801) | 0.248 |
| Urea (mg/dL) | 27.30 (9.95) | 30.87 (11.069) | 0.194 |
| Creatinine (mg/dL) | 0.820 (0.18) | 1.087 (0.42) | 0.003a |
DM: diabetes mellitus; BMI: body mass index; HDL: high-density lipoprotein.
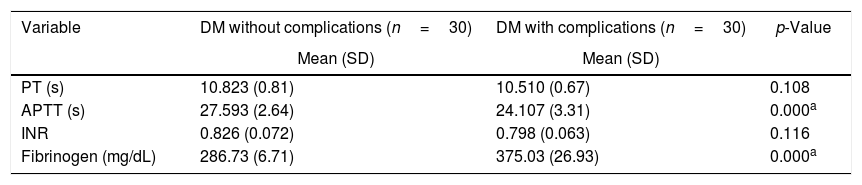
Comparison of coagulation profile of the diabetic patients with and without complications.
| Variable | DM without complications (n=30) | DM with complications (n=30) | p-Value |
|---|---|---|---|
| Mean (SD) | Mean (SD) | ||
| PT (s) | 10.823 (0.81) | 10.510 (0.67) | 0.108 |
| APTT (s) | 27.593 (2.64) | 24.107 (3.31) | 0.000a |
| INR | 0.826 (0.072) | 0.798 (0.063) | 0.116 |
| Fibrinogen (mg/dL) | 286.73 (6.71) | 375.03 (26.93) | 0.000a |
DM: diabetes mellitus; PT: prothrombin time; APTT: activated partial thromboplastin time; INR: international normalized ratio.
Statistical difference in coagulation parameters between diabetic patients with and without complications and control groups.
| Variable | Control (n=30) | DM without complications (n=30) | DM with complications (n=30) | F statistics | p-Value |
|---|---|---|---|---|---|
| Mean (SD) | Mean (SD) | Mean (SD) | |||
| Age (years) | 39.767 (14.8781) | 50.867 (9.7512) | 55.633 (7.4901) | 16.012 | 0.000a |
| PT (s) | 15.683 (4.8938) | 10.823 (0.8110) | 10.510 (0.6677) | 30.224 | 0.000a |
| APTT (s) | 36.207 (3.3332) | 27.593 (2.6378) | 24.107 (3.3122) | 120.229 | 0.000a |
| INR | 1.2060 (0.37619) | 0.8260 (0.07224) | 0.7980 (0.06343) | 31.007 | 0.000a |
| Fibrinogen (mg/dL) | 230.73 (17.322) | 286.73 (36.710) | 375.03 (26.933) | 200.719 | 0.000a |
DM: diabetes mellitus; PT: prothrombin time; APTT: activated partial thromboplastin time; INR: international normalized ratio.
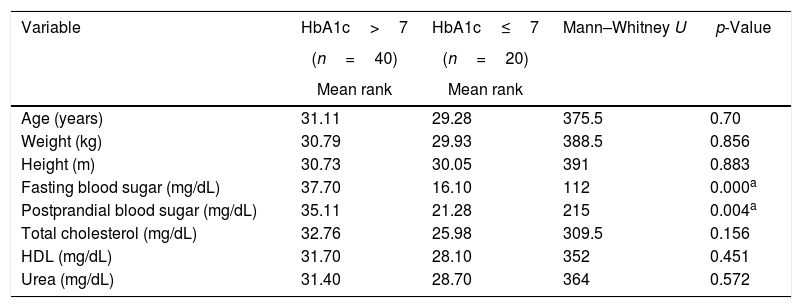
Comparison of clinical and biochemical parameters of diabetic patients according to HbA1c levels.
| Variable | HbA1c>7 | HbA1c≤7 | Mann–Whitney U | p-Value |
|---|---|---|---|---|
| (n=40) | (n=20) | |||
| Mean rank | Mean rank | |||
| Age (years) | 31.11 | 29.28 | 375.5 | 0.70 |
| Weight (kg) | 30.79 | 29.93 | 388.5 | 0.856 |
| Height (m) | 30.73 | 30.05 | 391 | 0.883 |
| Fasting blood sugar (mg/dL) | 37.70 | 16.10 | 112 | 0.000a |
| Postprandial blood sugar (mg/dL) | 35.11 | 21.28 | 215 | 0.004a |
| Total cholesterol (mg/dL) | 32.76 | 25.98 | 309.5 | 0.156 |
| HDL (mg/dL) | 31.70 | 28.10 | 352 | 0.451 |
| Urea (mg/dL) | 31.40 | 28.70 | 364 | 0.572 |
HDL: high-density lipoprotein.
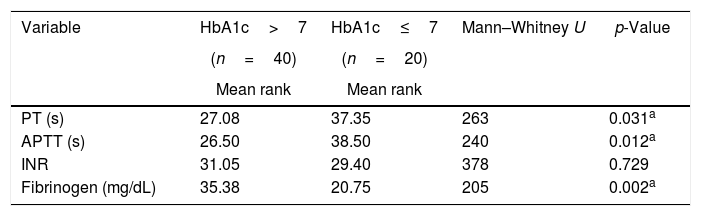
Coagulation profile of diabetic patients based on HbA1c.
| Variable | HbA1c>7 | HbA1c≤7 | Mann–Whitney U | p-Value |
|---|---|---|---|---|
| (n=40) | (n=20) | |||
| Mean rank | Mean rank | |||
| PT (s) | 27.08 | 37.35 | 263 | 0.031a |
| APTT (s) | 26.50 | 38.50 | 240 | 0.012a |
| INR | 31.05 | 29.40 | 378 | 0.729 |
| Fibrinogen (mg/dL) | 35.38 | 20.75 | 205 | 0.002a |
PT: prothrombin time; APTT: activated partial thromboplastin time; INR: international normalized ratio.
DM is a heterogeneous disorder that affects cellular metabolism in a variety of ways with coagulation parameters being severely affected.4 Hyperglycemia in diabetes contributes to hyperfibrinogenemia and activates the coagulative cascade, thus increasing thrombin formation and fibrinogen degradation products, which may stimulate hepatic fibrinogen synthesis. PT, APTT and fibrinogen tests are standard screening tests of coagulation system function and their utility in monitoring therapeutic anticoagulation is widely accepted.5
Diabetes is associated with increased risk of micro- and macro-vascular complications and is thus considered a procoagulant state.2 Increased fibrinogen levels are a strong and independent cardiovascular risk factor.
The purpose of this study was to investigate the coagulation abnormalities that lead to hypercoagulability in diabetes and to study their association with the development of complications.
In the present study, significant differences in age and duration of diabetes were observed between diabetic patients with complications and those without complications similar to the findings of other researchers such as Madan et al.2 and Dhwale et al.6 The present study also found significant correlations between age and duration of diabetes with and without complications and coagulation parameters such as APTT. However, Sapkota et al.7 found no significant association between APTT and duration of diabetes.
This study did not find any correlation of BMI with APTT levels similar to the study by Adonu et al.8 who reported that both lean and obese subjects with diabetes had reduced APTT values.
In the present study, the APTT was significantly lower and fibrinogen was significantly higher in type 2 DM patients with complications than those without complications however there was no significant difference in the PT. Similar to this study, Acang and Jalil9 observed that there were significant differences in all the coagulation parameters (higher fibrinogen levels, and shortened PT and APTT values) in diabetic patients, especially in patients with long-term diabetes and chronic complications. Carmassi et al.10 also found a significant difference but in a single parameter i.e. fibrinogen in diabetic patients with complications. On the contrary, Madan et al.2 did not find any significant difference in any of the coagulation parameters (PT, APTT and fibrinogen) between the two groups.
A statistically significant difference was found in age and all the coagulation parameters (PT, APTT, Fibrinogen) on comparing the three groups (diabetes without complications, diabetes with complications and controls) similar to several other studies in the literature.5,8,11 Similar to this study many other authors have found a significant increase in fibrinogen in diabetics compared to controls.3,6,12,13 In contrast Madan et al.2 found no significant difference in PT and APTT between diabetics and controls though fibrinogen showed a significant increase in diabetics. Sapkota et al.7 found that 73% of diabetics had APTT in the normal range though it was relatively shorter in the diabetic group compared to controls. However, in a study by Carmassi et al.,10 PT and APTT were found to be in the normal ranges in diabetics. In 1990, Van Wersch et al.14 observed increased fibrinogen concentrations in diabetic patients but the difference was not statistically significant in comparison with a control group. On the other hand, Alao et al.15 found significant increases in PT and APTT levels along with fibrinogen levels in diabetic patients compared to controls.
There was a significant difference in all of the coagulation parameters between diabetic patients with HbA1c≤7 and those with HbA1c>7 in accordance with the studies performed by other researchers.5,6
The major limitations of this study are the sample size and duration of the study. However, the authors understand that there could have been few unforeseen confounding factors that might have potentially influenced the results.
ConclusionClinical tests for PT, APTT and fibrinogen are relatively inexpensive and readily available. The present study shows that patients with DM and complications have lower PT and APTT values and higher fibrinogen levels than patients with DM without complications and non-diabetic controls.
Therefore it is indicated that shortened PT and APTT and increased fibrinogen levels might be useful hemostatic markers in diabetic patients, especially in those at high-risk for thrombotic complications. Further investigations of these markers could potentially be used as screening tests for hypocoagulable and hypercoagulable states that are applicable to diabetes and other clinical conditions.
Conflicts of interestThe authors declare no conflicts of interest.
Authors would like to thank Indian Council of Medical Research (ICMR), New Delhi for awarding a short-term studentship (STS) to Mr. Kashish Bansal, MBBS Student at ESIC Medical College, Faridabad, India.