The Zika virus (ZIKV) (genus Flavivirus, family Flaviviridae) is an arbovirus, but in addition to the mosquito bite, the virus can be also be transmitted by blood transfusion.1,2 Such a peculiar route of arboviral transmission is justified by the high rates of ZIKV asymptomatic infection in the affected population during outbreaks3 leading to the high prevalence of ZIKV viremia in blood donors.4,5 The objective of the present survey was to evaluate the ZIKV RNA prevalence among blood donations collected at the Blood Center of Brasilia, Federal District, Brazil during an extensive Dengue virus outbreak.
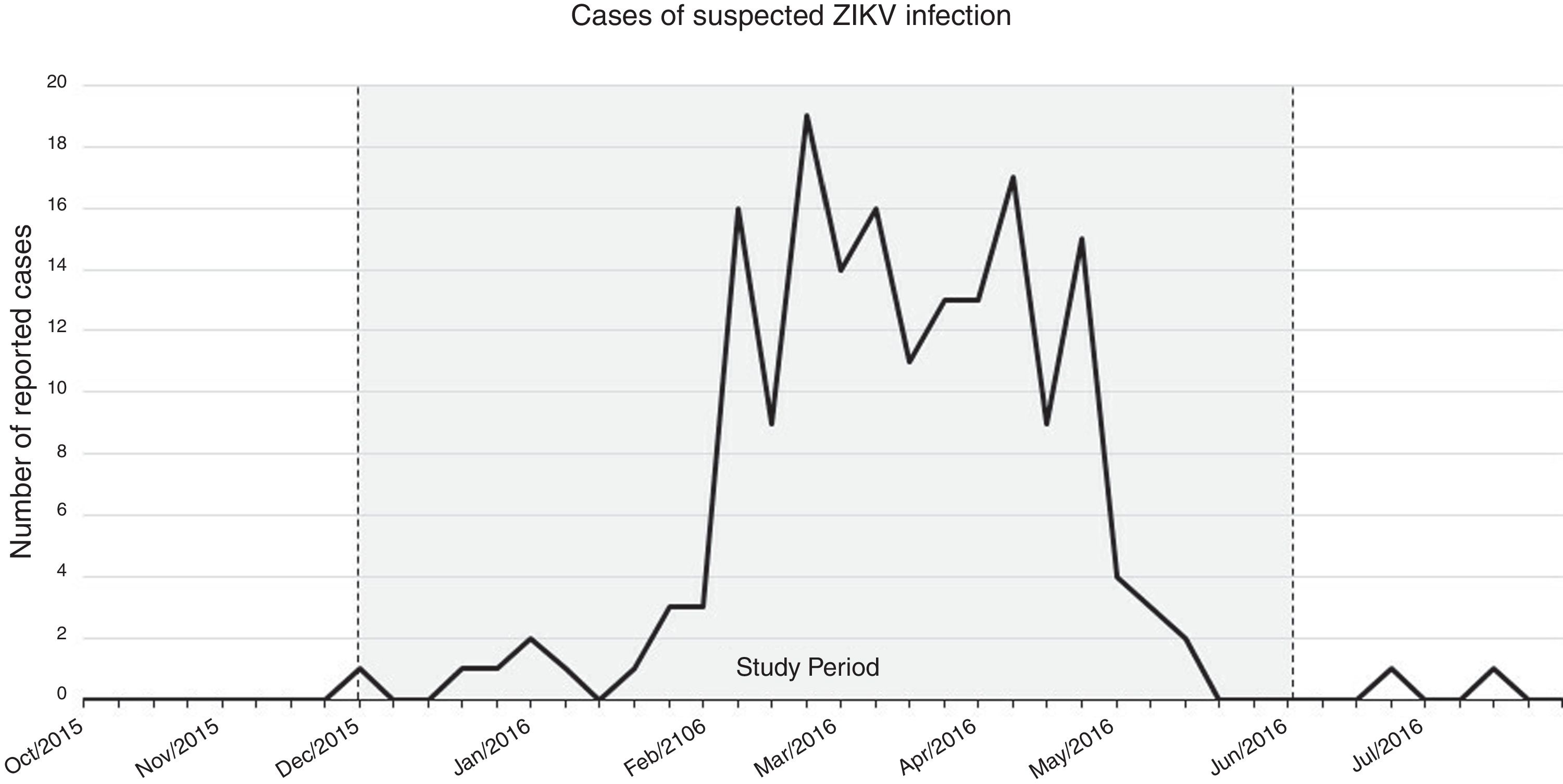
The peak of probable ZIKV cases in the general population of the Federal District of Brazil was observed between December, 2015 and May, 2016. During this period, 28,238 blood donations were obtained at the Blood Center of Brasilia, Federal District, Brazil. To calculate the appropriate sample size number to be tested in our study, an online epidemiology calculator was used (http://www.winepi.net/)6 (Confidence Interval: 95 %, desired precision ± 1 %). We adopted as a true estimated ZIKV prevalence the mean prevalence obtained from four previous studies examining ZIKV infection in Brazilian blood donors (0.71 %).5,7–9 The minimum sample size calculated to be tested for estimation of the ZIKV prevalence in blood donors was 269 donations; however, we tested a higher number of samples (475 blood donations).
Viral RNA was extracted automatically by the Maxwell 16 Viral Total Nucleic Acid Purification Kit (Promega) following the manufacturer’s instructions. The reverse transcription was performed using the High-Capacity cDNA Reverse Transcription kit (ThermoFisher Scientific) with specific reverse ZIKV primer. The detection of ZIKV RNA was performed by the TaqManⓇ real-time PCR, using a previously described molecular platform.10 Amplification was performed in an ABI 7500 real-time system (ThermoFisher Scientific).
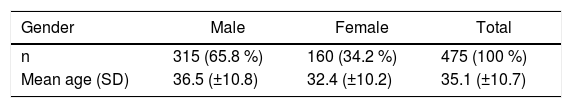
According to the Epidemiological Bulletin on Dengue, Chikungunya and Zika of the Federal District, Brazil, a greater number of probable ZIKV cases (777 cases) was reported in the general population between December 2015 and May 2016 (Figure 1). Of the 475 blood donations tested (Table 1), 315 (65.8 %) were obtained from male (36.5 ± 10.8 years old) and 160 (34.2 %) from female (32.4 ± 10.2 years old) blood donors. The performed real-time PCR demonstrated no positive results for ZIKV RNA. Considering the total number of blood donations in the study period (28,238), the performed statistical analysis demonstrated that the maximum ZIKV prevalence which can be expected was 0.627 % (CI: 95 %), or at least 2 ZIKV RNA positive donations.
In this pioneer study evaluating the ZIKV RNA prevalence among blood donors from the Blood Center of Brasilia, Central-West Brazil, we detected no positive results. The obtained results differ significantly from the ZIKV prevalence obtained for blood donors in the São Paulo State, Brazil5 and French Polynesia,4 where it was up to 3 %. On the contrary, our results were concordant with other studies performed in Brazil, especially in Northeast8 and South Brazil.9 where the detected ZIKV RNA prevalence was 0.0 %. In both studies, the authors claimed that the negative result might have been a consequence of the lower number of suspected ZIKV cases in the general population reported in the study period,8,9 compared to locations with large ZIKV outbreaks, such as São Paulo State. This situation can be similar to ours, in which only 777 probable ZIKV cases were reported by an epidemiological bulletin in the general population of the Federal District of Brazil. This might have contributed to the lower number of asymptomatic infections in blood donors and a negative PCR result in our study. During the study period, a higher DENV circulation was also reported as evaluated by the high anti-DENV IgM prevalence detected among blood donors,11 an infection which might have played a prominent role during the study period. Our results may also mean that when our study took place, the ZIKV outbreak may not have fully affected the Federal District of Brazil, thus differing from the ZIKV outbreaks reported in Southeast and Northeast Brazil. Although our results demonstrate that the risk of transfusion-transmission of ZIKV in the Federal District of Brazil can be considered very low in 2016, the performed investigation adds important information on the mode of ZIKV circulation during the Brazilian ZIKV outbreak and its impact on hemotherapy.
FundingThis project was financially supported by the Fundação de Apoio à Pesquisa do Distrito Federal, Federal District, Brazil - FAPDF (project number 0193000416/2016).
Conflicts of interestThe authors declare no conflicts of interest.