Essential thrombocythemia is one of the Philadelphia negative myeloproliferative neoplasms, characterized by persistent platelet count above 450 × 109/l, megakaryocytic hyperplasia, and presence of JAK2, CALR or MPL mutation.1 On the other hand, immune thrombocytopenia (ITP) is a diagnosis of exclusion, characterized by platelet count below 100 × 109/l, caused by production of anti-platelet antibodies, with the most common antibody target being the platelet glycoprotein IIb/IIIa complex.2 It can occur after viral infections, including hepatitis C virus (HCV), human immunodeficiency virus (HIV) and has also recently emerged as a complication of SARS-CoV-2 infection.3,4 To our knowledge, no case of ITP associated with SARS-CoV-2 infection in a patient with ET has been reported and only two case reports of ET with subsequent development of ITP were published, so far.5,6 Here we present a patient with ET, who developed ITP during the course of SARS-CoV-2 infection.
Case reportA 68-year-old man with history of essential thrombocythemia with JAK2 V617F mutation (missense point mutation with guanine to thymine transversion at position 1849 in exon 14 of the JAK2 gene, resulting in the exchange of valine for phenylalanine at position 617) diagnosed in 2000, chronically treated with 2 mg of anagrelide daily since 2010, with platelet levels above 200 × 109/l in past haematological check-ups tested positive for SARS-CoV-2 on 21st March 2021 and started to present mild clinical symptoms (headache, dry cough, mild fever) 3 days later.
The clinical symptoms gradually worsened, and the patient was examined in the Emergency Department 8 days after the positive polymerase chain reaction (PCR) test.
Upon arrival to Emergency Department on 29th March, a chest X-ray was performed and blood samples for complete blood count (CBC), serum biochemistry and coagulation testing were drawn. Laboratory findings were as follows: haemoglobin (Hb) 117 g/l, white blood cells (WBC) 5,22 × 109/l, platelets (PLT) 14 × 109/l with immature platelet fraction (IPF) 21,5%. Due to low PLT count, laboratory was unable to provide results for platelet parameters, such as mean platelet volume (MPV) and platelet distribution width (PDW).
Serum biochemistry and coagulation parameters (activated partial thromboplastin time, prothrombin time, fibrinogen) were unremarkable, except an isolated elevation of C-reactive protein (CRP) to 141 mg/l and elevation of d-dimers to 1700 µg/l (institutional reference range being <500 µg/l), which are common laboratory findings in SARS-CoV-2 associated pneumonia.7 The chest X-ray showed bilateral infiltrates, therefore according to institutional standards the patient was immediately admitted to the COVID-19 ward for i.v. administration of remdesivir and further investigation of grade IV thrombocytopenia.8
On admission to the COVID-19 ward, the patient´s SpO2 was 89%, body temperature was 38,5 °C, and the rest of the physical examination was unremarkable, with no signs of haemorrhagic manifestation nor mucosal bleeding. In order to further investigate the cause of grade IV thrombocytopenia, firstly his medical history was revisited. However, apart from essential thrombocythemia, it only included hypothyroidism on levothyroxine replacement therapy. New set of blood samples for CBC, peripheral blood smear, coagulation, serum biochemistry, infectious screening, autoimmunity screening, HLA-antibodies and antiplatelet antibodies were drawn and a CBC and CRP were drawn daily (Figure 1). In order to rule out myelodysplastic syndrome (MDS), acute myeloid leukaemia (AML) or lymphoproliferative disorders (LPDs) as an underlying cause of grade IV thrombocytopenia, a bone marrow aspiration with samples for flow cytometry, cytological evaluation, cytogenetics and fluorescence in situ hybridization (FISH) was performed.
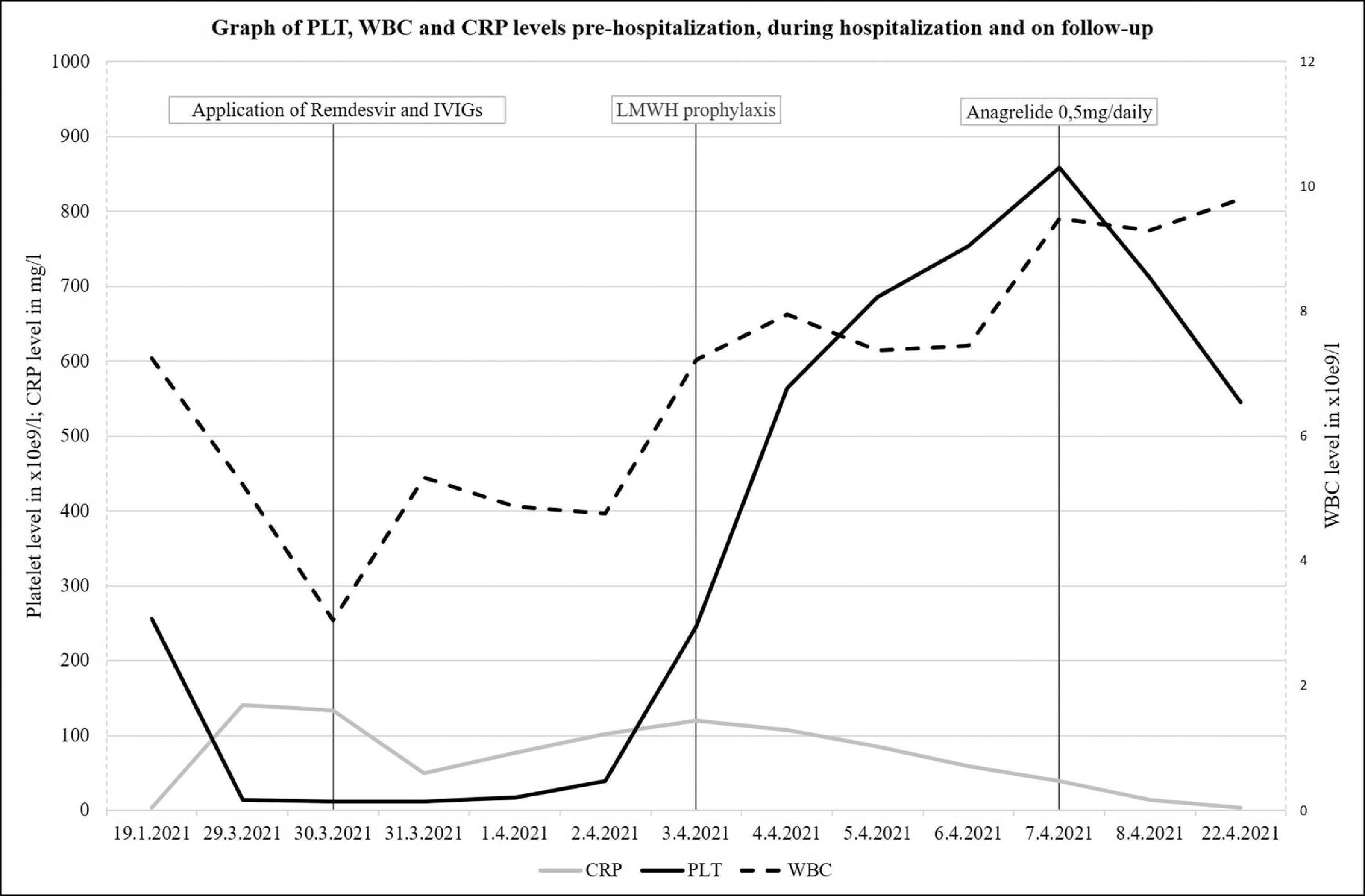
The line graph represents the evolution of PLT, WBC and CRP levels pre-SARS-CoV-2 infection, during the hospitalization and on the day of haematological check-up. Vertical lines represent particular milestones in the therapy: administration of remdesivir and IVIGs, LMWH prophylaxis and administration of anagrelide 0,5 mg/daily, respectively. Y axis on the left represents PLT and CRP levels and secondary Y axis on the right represents WBC levels.
On 30th March 2021, CBC showed a further decrease of the platelet level to 12 × 109/l with an increase in IPF to 26,2%. No dacrocytes, schistocytes nor myeloblasts were found on the peripheral blood smear evaluation. AML, MDS and LPDs were ruled out both by cytological evaluation and flow cytometry of the bone marrow aspirate. Cytological evaluation of one slide of the bone marrow aspirate only showed that 5 out of 21 megakaryocytes were smaller and with hypo lobulated nuclei and an increase in segmented neutrophiles was observed. Cytogenetics and FISH results showed no chromosomal aberrations typical for MDS or AML. Both serological screening for human immunodeficiency virus, hepatitis C virus, hepatitis B virus, hepatitis A virus, cytomegalovirus, herpes simplex virus, Mycoplasma species, Helicobacter pylori, screening of autoimmune diseases and HLA antibodies were negative. Tests for antiplatelet antibodies returned positive, with an antibody against glycoprotein complex IIb/IIIa identified by indirect immunofluorescence. Combined clinical and laboratory findings were interpreted as ITP secondary to SARS-CoV-2 infection.
Immediately upon admission on 29th March, anagrelide was discontinued, patient received one unit of platelet concentrate, intravenous antipyretic medication and according to institutional standards also 8 mg intravenous (i.v.) dexamethasone was administered. On 30th March, 5-day treatment of remdesivir and second dose of 8 mg i.v. dexamethasone were instituted. For ITP treatment, a 4-day course of intravenous immunoglobulins (IVIGs) 0,5 g/kg was added. After the administration of IVIGs the platelet count began to rise, reaching 246 × 109/l on 3rd April, therefore low-molecular-weight-heparin (LMWH) prophylaxis with enoxaparin was started. (Figure 1) On account of further increase of the platelet level to 858 × 109/l, with MPV 10,2fl and PDW 10,7fl on 7th April, anagrelide was returned to chronic medication in a dose of 0,5 mg daily. The patient was discharged from the ward on 8th April, fully recovered from SARS-CoV-2 associated pneumonia, with haematological follow-up arranged two weeks after discharge. Upon planned haematological check-up on 22th April, samples for CBC, serum biochemistry, SARS-CoV-2 antibodies and anti-platelet antibodies were drawn. Results were as follows: PLT level decreased to 545 × 109/l, MPV was 9.9 fl, PDW was 10.2 fl, Hb was 118 g/l, WBC 9,80 × 109/l, CRP was below 4 mg/l, serum biochemistry was unremarkable, both IgM and IgG anti-S-2019-nCov exceeded the cut-off level of 1,0 AU/ml and anti-gpIIa/IIIa were negative.
DiscussionEssential thrombocythemia is a myeloproliferative disease of bone marrow hematopoietic stem cells characterized by acquired somatic mutations, which provide a selective advantage to mutated cells over the normal hematopoietic stem cells and this condition results in indefinite self-renewal of the neoplastic clone.1 Even though ET can transform into MDS or AML in approximately 1–5% of cases, in this patient the bone marrow evaluation and increased immature platelet fraction in the peripheral blood showed, that transformation to AML or MDS was not the underlying cause of the thrombocytopenia.9 Although, the most common symptoms seen in patients with SARS-CoV-2 infection are fever, fatigue, dry cough and gradually developing dyspnoea, haematological changes are also commonly observed, including prolonged thromboplastin time, elevation of d-dimers, lymphopenia and thrombocytopenia.7 In the case of this patient, three possible causes of SARS-CoV-2 associated thrombocytopenia were considered in the differential diagnosis: ITP, thrombotic thrombocytopenic purpura (TTP), and disseminated intravascular coagulation (DIC).3,10,11 Heparin induced thrombocytopenia (HIT) was not taken into consideration in the differential diagnosis, as the patient did not receive any heparin nor LMWH before the development of thrombocytopenia.12 As the coagulation studies, except for elevation of d-dimers, were normal, and no schistocytes nor dacrocytes were present in the peripheral blood smear, both TTP and DIC were ruled out.10,11 The diagnosis of ITP was made based on combined clinical and laboratory findings, including high immature platelet fraction and prompt increase in platelet level after administration of intravenous immunoglobulins. Presence of anti-gpIIa/IIIb antibodies also supported the diagnosis.2
In conclusion, we report a case of a patient with ET, who developed ITP during the course of SARS-CoV-2 infection, suggesting that immune-mediated platelet destruction has the ability to overcome the mutated megakaryocytic cell line.5,6
Statement of contributionAcquisition of data: B.B., L.G., M.M., I.Z., Analysis and interpretation of data: B.B., T.K, J.N., Treatment of patient: B.B., L.G., M.M., I.Z., Drafting of manuscript: B.B., J.N. All authors revised and approved the final version of the manuscript.