We report a case of corona virus disease 2019 (COVID-19) positive 58-year female patient who presented with complaints of fever and cough for the past 3 days. She was a known case of Diabetics mellitus and hypertension for 3 years. She then underwent COVID-19 testing by RT-PCR method and was positive. Complete hemogram sample was also collected simultaneously to look for viral changes.
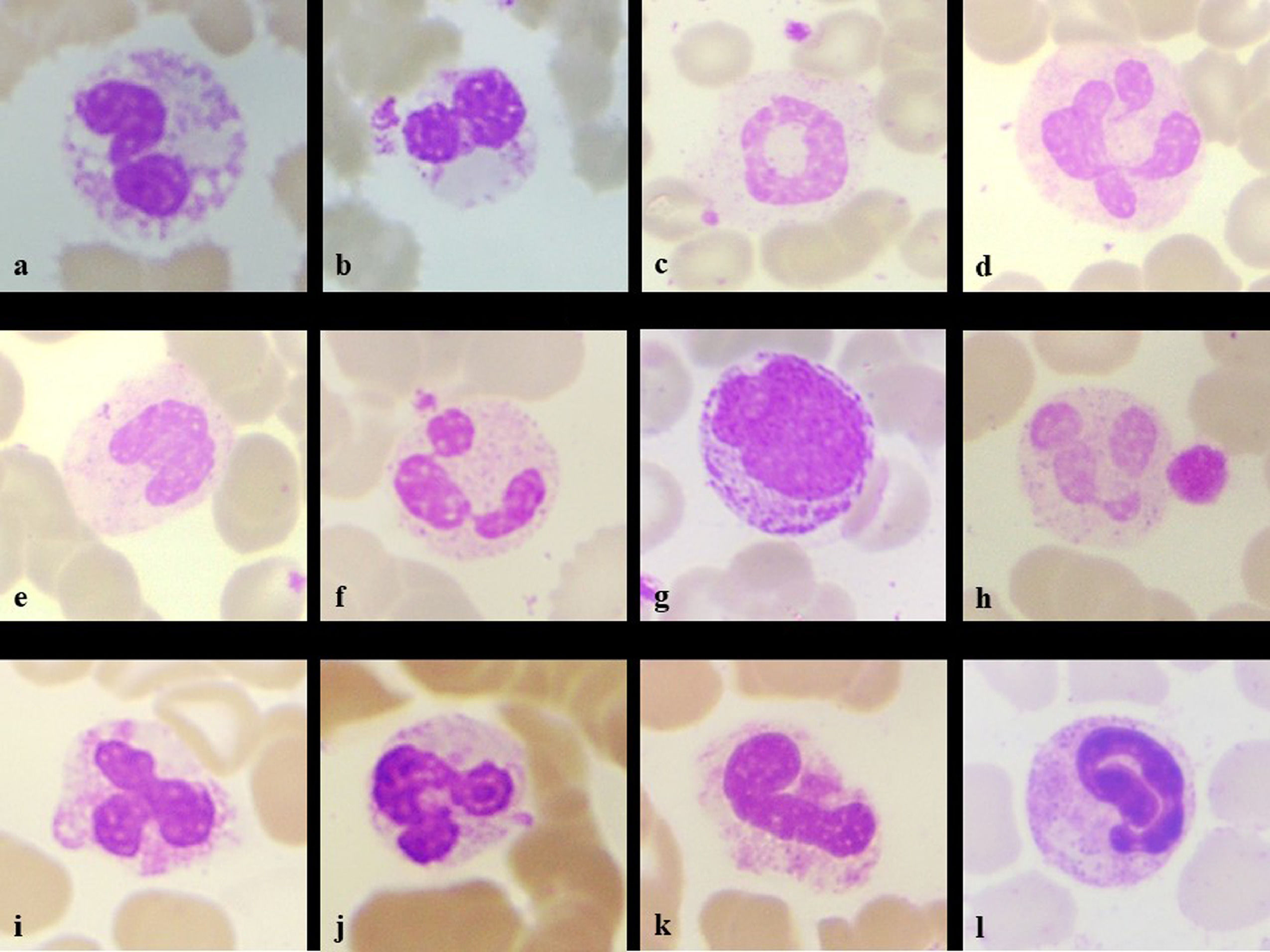
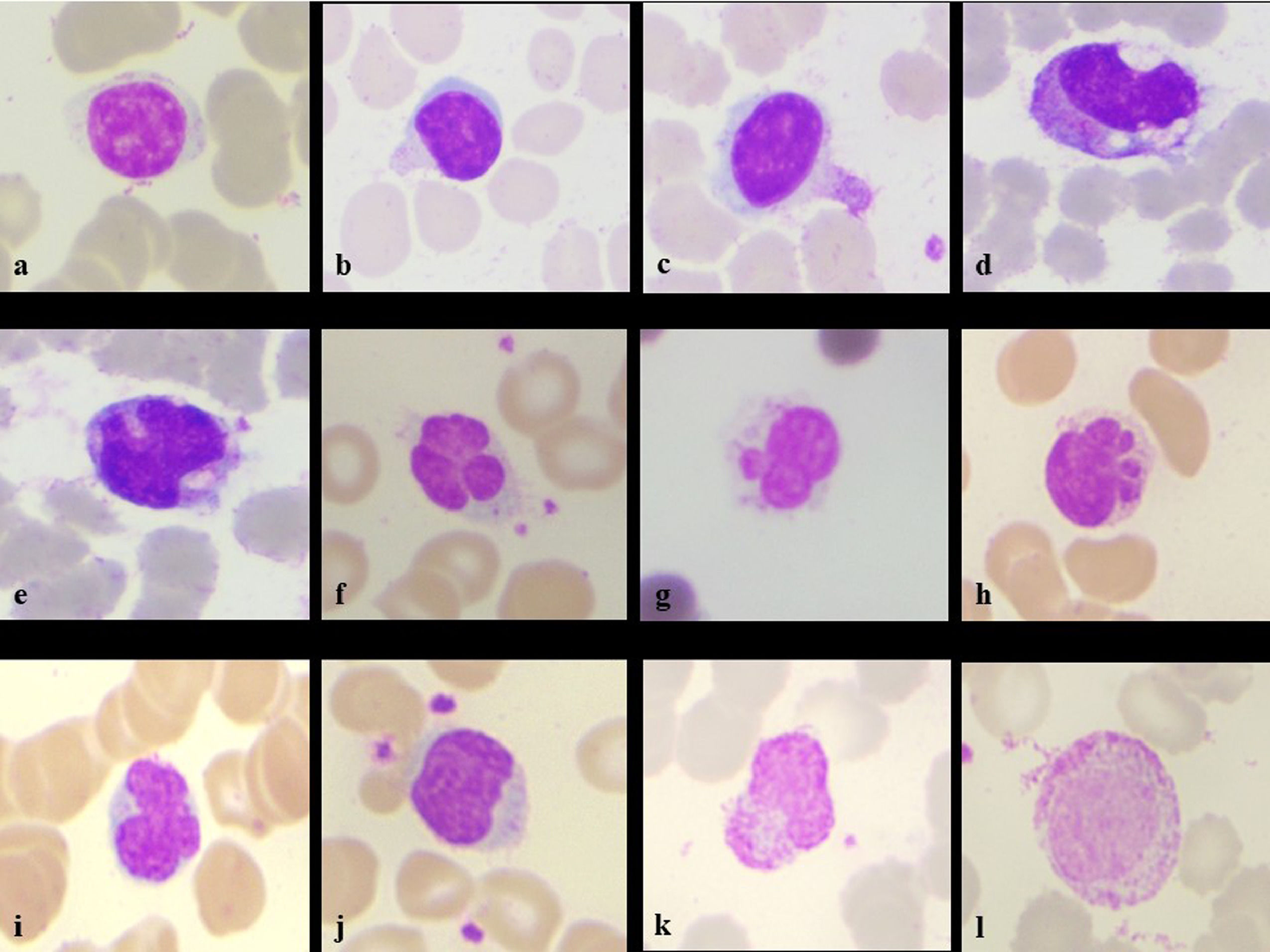
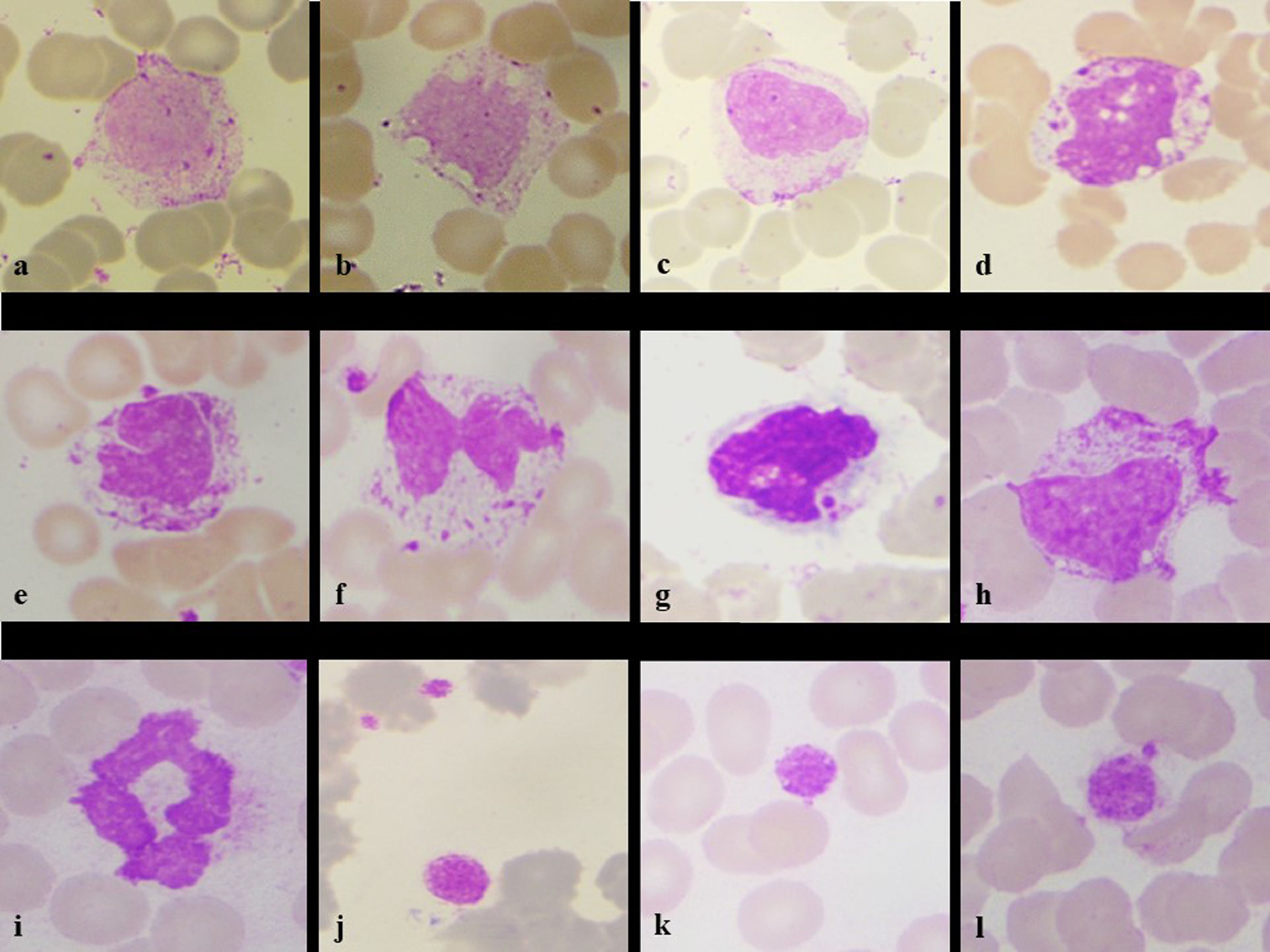
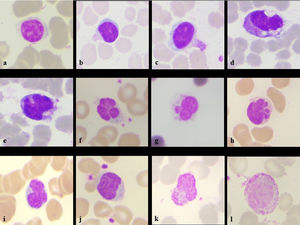
Her hemoglobin was 9.1g/dL, platelet count of 327 × 103/µL and total leucocyte counts of 14,500/mm3, Differential counts revealed- neutrophil 85%, lymphocyte 07%, monocyte 05%, eosinophil 00%, basophil 00%, band form 01% & myelocyte 02%. Peripheral smear revealed the normochromic normocytic blood picture with mild shift to left. There were morphological alterations in leucocytic lineages- Neutrophils showing the features of nuclear hypo segmentation, ring shape, club shape, "U" shape, fetal like, hypo granulation, satellitism. (Figure 1a-l). Lymphocytes showing cytoplasmic pods, vacuolations, nuclear blebbing, outpouchings, increased granulation in large lymphocytes (Figure 2a-l). Monocytes having abundant cytoplasm with granulations, vacuolations, nuclear blebbing's, irregular cytoplasmic membranes. Smudge cells, giant platelets and platelet satellitism were also seen (Figure 3a-l). The patient was kept in isolation ward and discharged on the completion of 14 days of isolation without any other symptoms.
Neutrophil changes seen in the patient- intracytoplasmic vacuoles (a), pseudo-Pelger-Huet nuclei (b), ring (c), clubbed (d), monolobated (e), drumstick with platelet satellitism (f), myeloid precursor (g), hypo granulation with giant platelet (h), tripolar (i), "U" shape (j), fetus like (k), elongated nucleoplasm (l) (Leishman stain, x100)
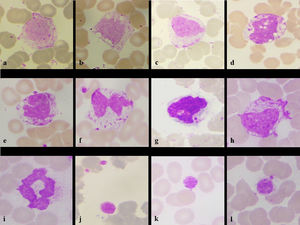
Lymphocyte morphological changes seen in the patient- normal small lymphocyte (a), cytoplasmic outpouching (b), cytoplasmic pod (c), plasmacytoid lymphocyte with cytoplasmic vacuoles (d), in-folding of nucleus (e), nuclear blebs with platelet satellitism (f,g), multiple blebs/baby feat (h), nuclear lobations (i), irregular nuclear membrane with platelet satellitism (j), cytoplasmic pod and granularity (k), large lymphocyte with increased granularity (l) (Leishman stain, x100)
Monocyte showing irregular cytoplasm outline (a), cytoplasmic vacuolation (b), nuclear bleb (c), intracytoplasmic and intranuclear vacuolation (d), horse shoe nuclei (e), bilobed and platelet satellitism (f), engulfed platelet (g), increased cytoplasmic granularity (h), ring shaped smudge cells (i), and platelet changes in form of giant platelets (k) and platelet adhesion (l). (Leishman stain, x100)
Peripheral smear with neutrophilia, lymphopenia, smudge cells, thrombocytopenia, etc. can be seen in patients with COVID-19 positive. Morphological features such as myeloid left shift, atypical reactive lymphoid changes, giant platelets and fragmented or smudged neutrophils, C- shaped, fetus like, ring and elongated nucleoplasm are some of the highly sensitive morphologic changes which can be noted in COVID 19 patients.1-3
The inflammatory response and viral effect can be seen in the leucocytic morphology changes. Monocytes along with activated macrophages have a favorable prognosis. Lymphopenia and eosinopenia indicates the disease progression and severity. The peripheral smear can be used as a basic screening technique while the reports of RT-PCR are awaited and used for treatment follow up changes.1-3