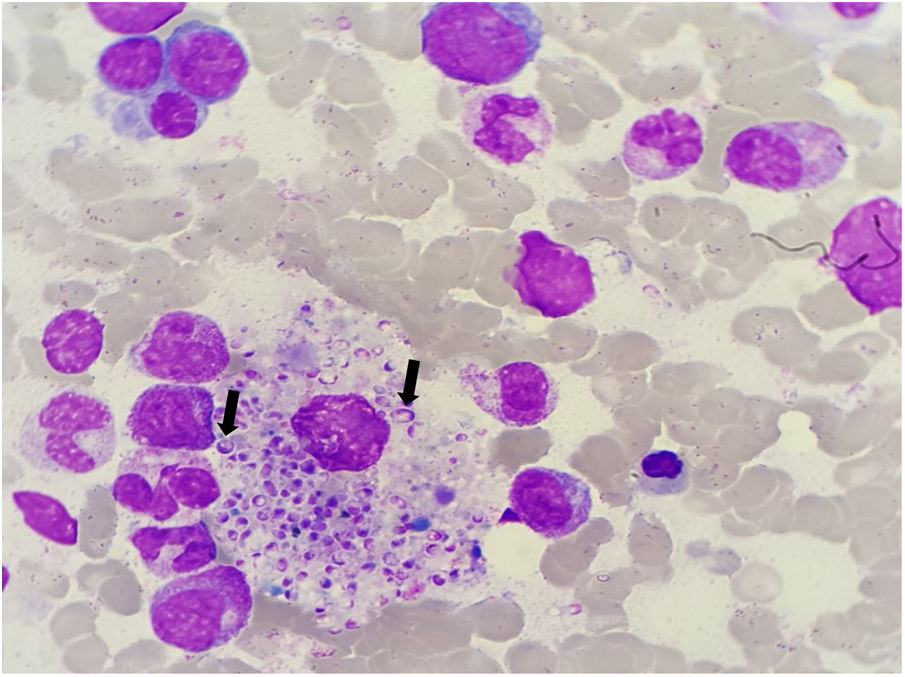
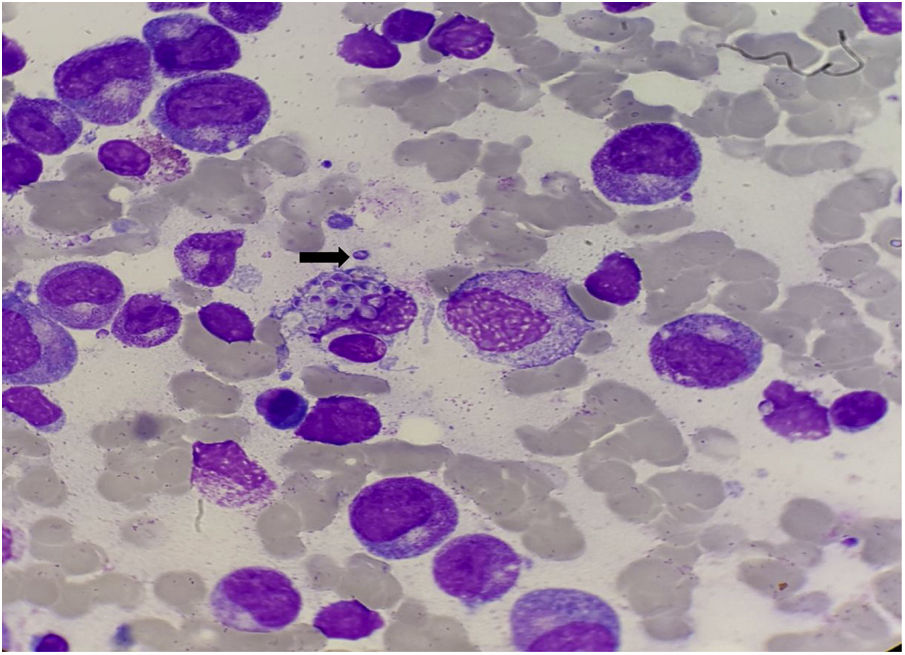
Histoplasmosis is a fungal infection caused by a dimorphic fungus Histoplasma capsulatum.1 Progressive disseminated histoplasmosis (PDH) is an AIDS-defining illness with a high lethality rate if not promptly treated.3 In patients with disseminated disease, culture and pathology are the most sensitive.2 The gold standard for the identification of the pathogen is the culture demonstrating the thermal dimorphism of the fungus.3 We present a case of a 52 year old male with HIV-1 infection (CDC-C3) and a recent trip to Brasil, admitted in the ICU with a diagnosis of Pneumocystis jirovecii pneumonia (under co-trimoxazole treatment) and haemophagocytic lymphohistiocytosis. A bone marrow (BM) aspirate was performed and stained May-Grunwald-Giemsa films revealed numerous yeast-like bodies inside and outside macrophages with morphology suggestive of Histoplasma spp (Figure 1 and 2). Culture and molecular results (bone marrow PCR) confirmed the microbiological diagnosis- Histoplasma capsulatum.
The author declares no conflicts of interest.